‘Periodontal disease is a major public health problem associated with oral bacteria, as it could be a risk factor for cardiovascular disease, diabetes, and other chronic health conditions.’
Tweet it Now
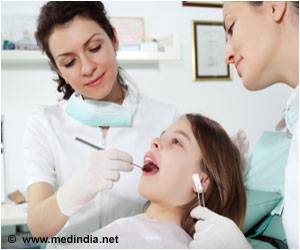
Periodontitis is diagnosed by measuring the depth of the pockets in the gums next to the teeth. "But diagnosing periodontitis visually is impossible and it doesn't usually give any symptoms until it has developed so far that teeth become mobile, which is very late for any treatment," said coauthor Ulla Harjunmaa, a dentist with a master's degree in International Health, who is a PhD student at the Center for Child Health Research, University of Tampere and Tampere University Hospital, Finland. Diagnosis requires specially trained dental professionals and expensive equipment, which are seldom available in developing countries, said Harjunmaa. But among other things, in the future, this research may lead to an inexpensive and rapid point-of-care test, based on distinguishing the two conditions' microbiomes. "The research made it possible to tell which differences in bacteria were linked specifically to the deepening of dental pockets--which causes loss of teeth--rather than just to bleeding gums," explained Shaw.
"We're not the first to do this sort of research into the periodontal disease, but our study is the largest to be done in such a setting," said Shaw. "There is a great need to find new solutions to prevent these problems everywhere, but especially in this kind of setting." He added that oral infections are very common in Malawi, since there is little awareness about oral health and prevention, and little treatment available.
Some of the techniques used in the research may have wide applications, said Shaw. "Where diseases can have multiple severities and clinical features that are also found in non-disease (like bleeding gums in periodontitis), this kind of modeling will be increasingly important in microbiome research."
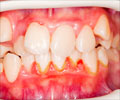
Periodontal disease is a major public health problem associated with oral bacteria. In developed nations, approximately half of adults are thought to have the moderate periodontal disease, with another 7-15 percent having advanced disease, according to the Centers for Disease Control and Prevention. Additionally, periodontal disease is thought to be a risk factor for cardiovascular disease, diabetes, and other chronic health conditions. Treating gum disease could reduce healthcare costs, as well as hospitalizations, according to a study published in August 2014 American Journal of Preventive Medicine.
Advertisement
The research is published in the Applied and Environmental Microbiology, a journal of the American Society for Microbiology.
Advertisement