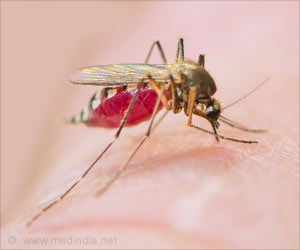
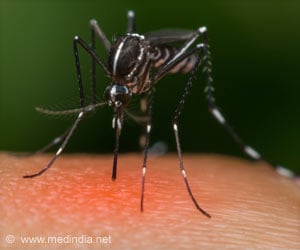
‘Exposure to the latter blood stage of malaria infection inhibits the formation of the protective immune cells (and their antibodies) that can prevent the early liver stage infection.’
Tweet it Now
"The blood stage of malaria infection has a very profound impact on
the liver stage immune response, and that impact had never been
dissected and visualized at this level," says co-author Marion Pepper,
UW Medicine researcher and assistant professor of immunology at the UW
School of Medicine. "These studies really suggest that you need a
vaccine that is protective against both stages of infection to
effectively prevent malaria."To track how the blood stage of malaria infection overpowers the liver stage immune response, Pepper and her collaborators infected two groups of mice with different forms of the malaria parasite. One of these was engineered by their collaborators in the lab of Stefan Kappe, UW affiliate professor of global health and investigator, Center for Infectious Disease Research in Seattle, to stop at the liver stage of infection, while the other progressed to the blood stage of infection.
Six days after infection, the researchers found that the levels of antibodies were significantly lower in the mice with the blood stage infection than in mice that only had the parasite targeted to the liver.
To understand this discrepancy, the team tracked the differentiation of Plasmodium liver stage-specific B cells. B cells can differentiate into antibody-secreting early effector cells or long-lived memory cells, both of which contribute to protection against malaria.
They discovered that 14 days after infection, the B cells in the blood stage infected mice never went through the necessary changes to make rapidly responsive memory cells. However, in the mice that received the liver-stage attenuated version of the parasite, the B cells were still able to differentiate and create the necessary antibodies and memory cells for an effective immune response.
Advertisement
Pepper and her collaborators are now looking into the possibility of a drug treatment to solve this problem, as they were able to show that when you treat the second stage of the infection with a drug, the B cells are able to create the optimally responsive memory cells. But for now, the researchers are hopeful that their work can be used to answer immediate questions about the efficacy of malaria vaccines in regions that are most significantly affected by the disease.
Advertisement
Source-Eurekalert