Before their work only a few such genes were known. The findings could eventually lead to new ways to stop malaria parasites before people get sick and help keep the disease from spreading, via treatments that are less likely to promote resistance than existing malaria drugs, the researchers say.
The study appears online in the journal Cell Chemical Biology.
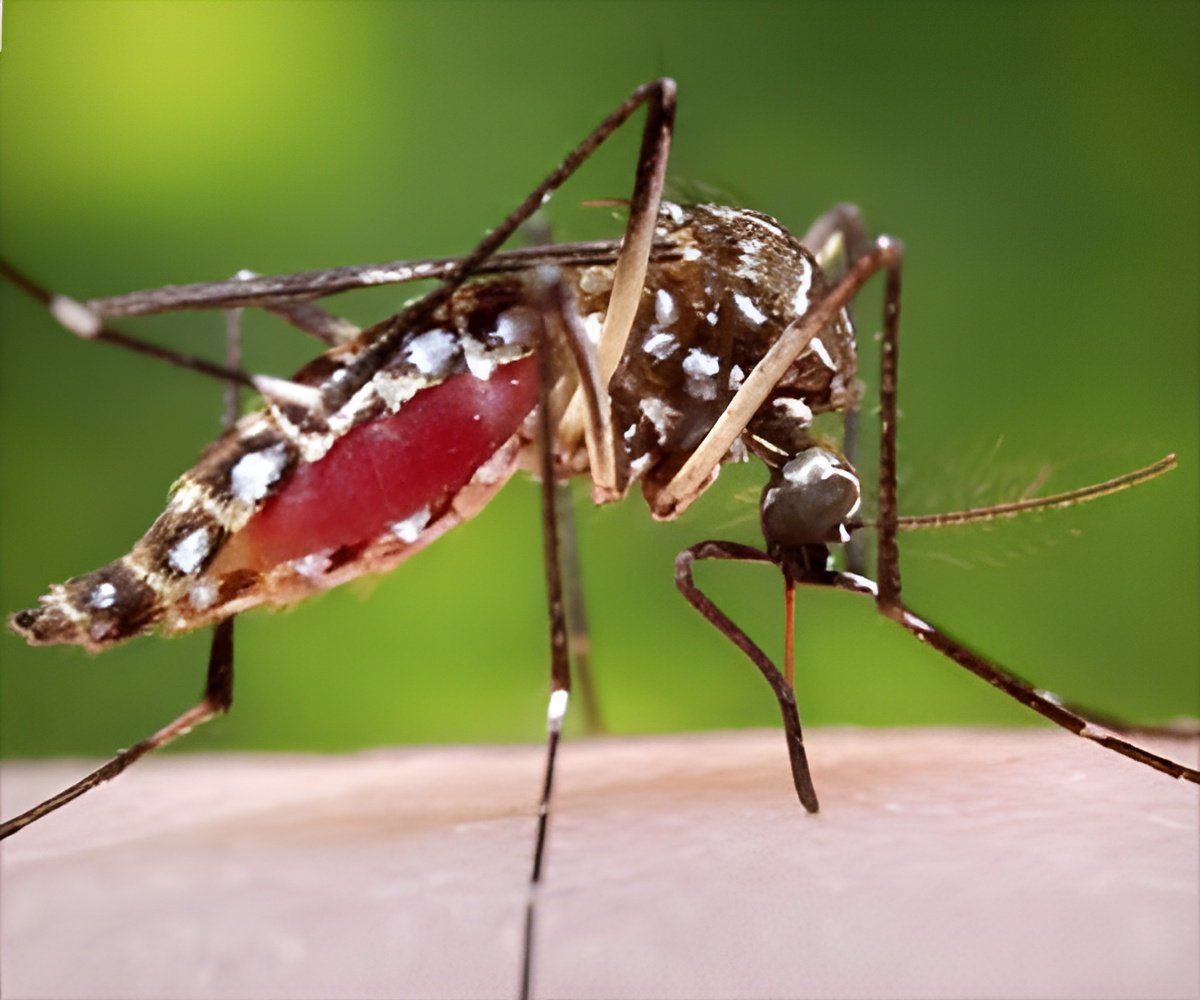
Malaria is caused by Plasmodium, a single-celled parasite spread through the bites of infected mosquitoes. Within hours of entering a person's body, the parasite finagles its way into a liver cell, which it uses as a sort of living nursery. There, it steals bits of the host's cell membrane to help build a protective pouch inside the cell where it quietly matures and multiplies before bursting out by the thousands into the bloodstream.
That's when the parasite starts to invade red blood cells and cause malaria's characteristic waves of fever and chills. The blood stage is also when parasites can be picked up by another biting mosquito and transmitted to the next person. If we could stop the parasite while it still lurks in the liver, before it reaches the blood, researchers say, we could keep people from developing symptoms or contributing to its spread.
For this study, researchers used snippets of silencing RNA to trick human liver cells into tamping down each of roughly 7,000 protein-coding genes. Then they infected the liver cells with a mouse malaria parasite similar to the Plasmodium species that causes human malaria. The researchers looked to see if, by preventing the cells from making a given protein, they could reduce the parasite load within the liver without killing the liver cells themselves.
Advertisement
"Many of the drugs that are available aren't working very well because of resistance," Derbyshire said.
Advertisement
"Even though tens of thousands of parasites come out of the liver, that's still a very small number compared to the billions that build up later in the blood stage," said co-first author Maria Toro-Moreno, a chemistry graduate student at Duke.
This choke point could make for an easier target, Toro-Moreno explained. "It's a population bottleneck. The parasite is vulnerable at this stage."
Lower numbers also mean the parasites in an infected person's body are less genetically diverse. A drug administered at this stage is less likely to promote resistance than one administered after Plasmodium has multiplied more, during which time random genetic mutations could arise that enable some parasite strains to survive treatment.
Identifying potential targets is just a first step in drug development, a process that can take over a decade and require millions of dollars of investment before reaching the clinic. But by better understanding the intimate relationship between the malaria parasite and its host, the researchers hope to get closer.
Source-Eurekalert













