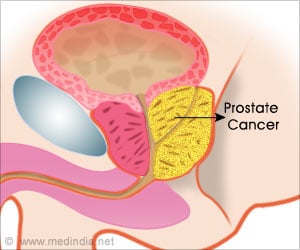
In people with prostate cancer, a radical prostatectomy is often called for in which the prostate gland and some of the surrounding tissue is surgically removed.

‘Benefits of light reflectance spectroscopy include highly accurate surgical removal of all cancerous tissue and the ability to spare more healthy tissue, minimizing the likelihood of cancer recurrence.’





"We used a novel light reflectance spectroscopy probe to evaluate surgical margins on radical prostatectomy tissue specimens and correlated the findings with pathological examination," said Dr. Jeffrey Cadeddu, Professor of Urology and Radiology at UT Southwestern and lead author of the study, which was published recently in the the Journal of Urology. Light reflectance spectroscopy measures light intensity reflected or backscattered from tissues. When someone has prostate cancer, a radical prostatectomy is often called for in which the prostate gland and some of the surrounding tissue is surgically removed. Due to the amount of time involved with traditional techniques and the lack of proven clinical usefulness, analysis to determine removal of all cancer surrounding the visible tumor's edges is not routinely performed during surgery. As such, undetectable cancer cells can be left behind and are termed "positive surgical margins."
Patients with intermediate- to high-risk disease requiring radical prostatectomy were enrolled in the study. Immediately after the prostate gland was removed, light reflectance spectroscopy was performed on suspected malignant and benign prostate margins. Each sample was analyzed and correlated with pathological samples, which were analyzed post-surgery. Light reflectance spectroscopy analysis was performed on 17 prostate gland specimens, on which a total of 11 histologically positive and 22 negative surgical margins were measured. The optical probe predicted positive surgical margins with 85 percent sensitivity, 86 percent specificity, and 86 percent accuracy.
"This study highlights one of a growing number of technology platforms that aim to improve the outcomes of cancer surgery," said Dr. Cadeddu, who holds the Ralph C. Smith, M.D., Distinguished Chair in Minimally Invasive Urologic Surgery. "Further study is required to determine whether such analysis may be used in real time to improve surgical decision-making and decrease the amount of tissue surgeons need to remove."
According to the National Cancer Institute (NCI), prostate cancer is the most common cancer in men, second only to skin cancer. After lung cancer, prostate cancer is the second leading cause of cancer-related deaths in U.S. males. NCI estimated that 220,800 men would be diagnosed with prostate cancer in 2015, and nearly 27,540 men would die of the disease - the most recent data available.
Advertisement
The Harold C. Simmons Comprehensive Cancer Center is the only NCI-designated Comprehensive Cancer Center in North Texas and one of just 45 NCI-designated Comprehensive Cancer Centers in the nation. The Simmons Comprehensive Cancer Center includes 13 major cancer care programs with a focus on treating the whole patient with innovative treatments, while fostering groundbreaking basic research that has the potential to improve patient care and prevention of cancer worldwide. In addition, the Center's education and training programs support and develop the next generation of cancer researchers and clinicians.
Advertisement
Source-Eurekalert






![Prostate Specific Antigen [PSA] Prostate Specific Antigen [PSA]](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)