Those with OA experience painful swelling and stiffness of the joints such as knees, hips and fingers. The National Arthritis Data Workgroup estimates that 27 million Americans over 25 years of age have OA (based on 2005 U.S. census data). A long-term study by researchers from the University of North Carolina—the Johnston County OA Project—suggests that lifetime risk of developing knee OA is roughly 46%.
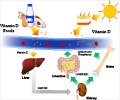
During the last decade medical evidence has uncovered the importance of vitamin D, not only as a vitamin that aids in calcium absorption, but as a powerful hormone with numerous functions throughout the body. In fact, studies have found that a decreased vitamin D level reduces immunity and may contribute to diseases such as cancer and diabetes.
Most vitamin D in humans comes from exposure to the sun, with research suggesting that a deficiency of this important vitamin may be due to more indoor activities, increased sunscreen use, and need for longer sun exposure for those with dark skin pigmentation. One study estimates that 95% of black Americans compared to 70% of white Americans have low levels of vitamin D.
"People associate vitamin D with good bone health," said lead author Toni Glover, MSN, ARNP, a research nurse practitioner and doctoral candidate at the University of Florida, specializing in the study of pain in older adults. "Yet, not everyone is aware of what factors decrease vitamin D and how low levels could contribute to health issues, including chronic pain."
Clinical practice guidelines state that vitamin D levels less than 20 ng/mL represent deficiency and levels between 21 and 29 ng/mL represent insufficiency. Given that low levels of vitamin are linked to chronic pain and other health conditions, especially in black Americans, the research team set out to investigate if variations in vitamin D levels contribute to racial differences in patients with knee pain caused by OA.
Advertisement
In addition, study subjects underwent testing that included sensitivity to heat and mechanical pain on the affected knee and the forearm. Researchers measured heat pain threshold as the point when patients indicate the sensation "first becomes painful" and pain tolerance when patients "no longer feel able to tolerate the pain." Mechanical pain measures were determined by the patients' response to pressure in the knee and forearm.
Advertisement
"Our data demonstrate that differences in experimental pain sensitivity between the two races are mediated at least in part by variations in vitamin D levels," concludes Ms. Glover. "However, further studies are needed to fully understand the link between low vitamin D levels and racial disparities in pain. Although rare, vitamin D toxicity is possible and older adults should consult with their primary care provider regarding supplementation. It may be warranted that older black Americans with chronic widespread pain be screened for vitamin D deficiency to reduce disparities in pain." The authors plan to pursue additional research which tests the impact of improving vitamin D status on chronic pain for older black and white Americans.
Source-Eurekalert