"Finding the optimal conditions to avoid interfering with immune cells working to eradicate cancer while preventing graft rejection and GVHD is the holy grail of bone marrow transplant," says Leo Luznik, M.D., associate professor of oncology at the Johns Hopkins Kimmel Cancer Center. "We've known for some time that giving cyclophosphamide after a transplant helps prevent GVHD, and our study provides an important piece of the puzzle for why it works."
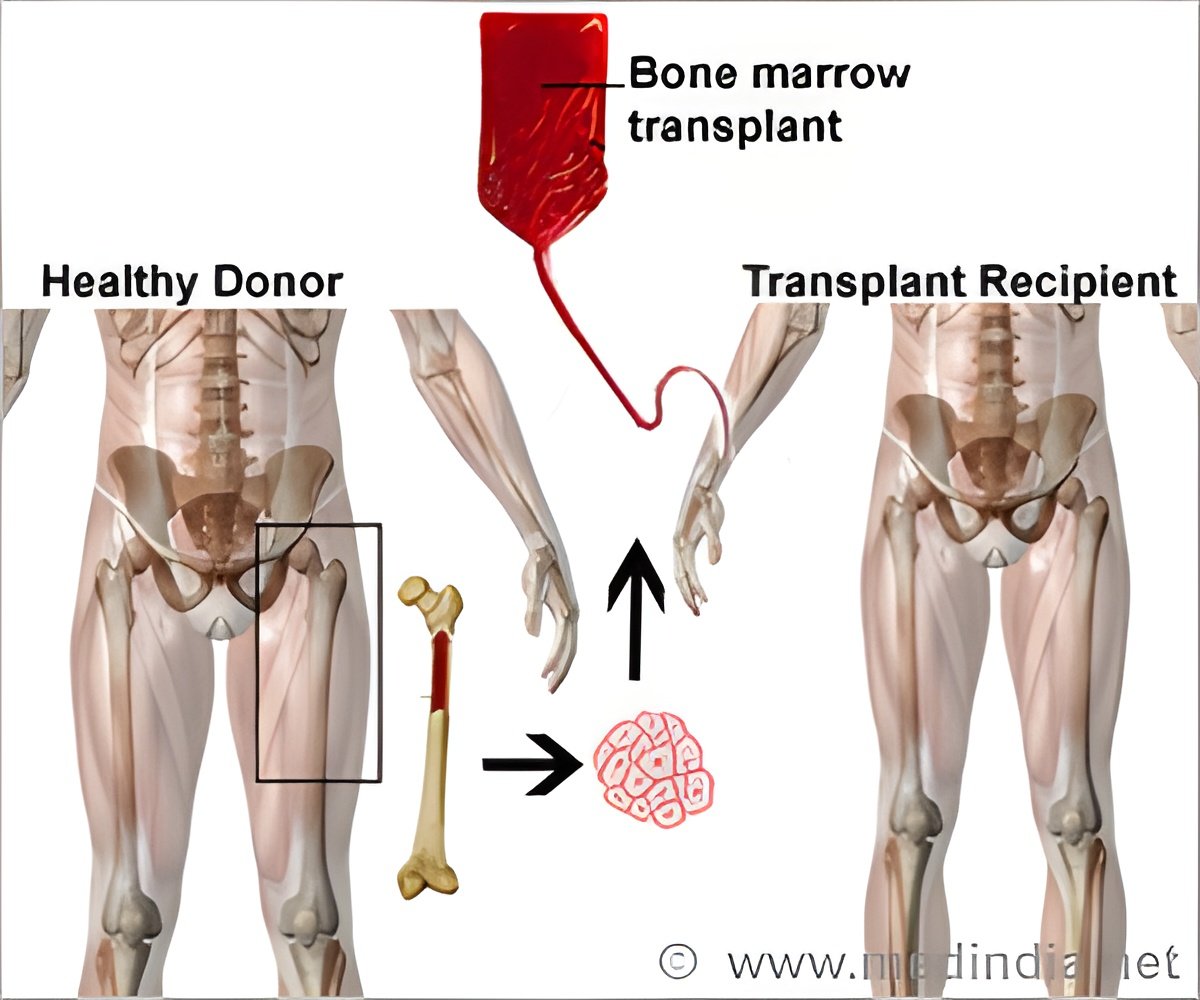
GVHD occurs when newly transplanted immune cells from a donor's bone marrow attack the patient's body. Commonly used immunosuppressant drugs prevent rapid-onset, acute GVHD but not persistent, long-lasting, chronic GVHD, which may cause severe disability and death.
In the early 2000s, Johns Hopkins scientists Leo Luznik and Ephraim Fuchs found that giving patients high doses of cyclophosphamide - a drug derived from nitrogen mustard and used to treat blood cancers - three days after bone marrow transplant successfully thwarts acute and chronic GVHD. Johns Hopkins physicians also found that post-transplant cyclophosphamide enabled safe administration of new, half-matched bone marrow transplants in addition to traditional, fully matched ones. Medical centers around the world now use the Johns Hopkins protocol of post-transplant cyclophosphamide, and Luznik says the inexpensive drug is becoming increasingly mainstream in bone marrow transplant regimens.
Some of the first clues to how cyclophosphamide works were also discovered in the 1980s by Johns Hopkins scientists. They found that cyclophosphamide kills all of the donor's transplanted bone marrow cells except for stem cells containing high levels of an enzyme called aldehyde dehydrogenase (ALDH). The ALDH-laden stem cells evade the toxic effects of cyclophosphamide and rebuild the patient's immune system. Richard Jones, M.D., professor and director of the Bone Marrow Transplant Program at Johns Hopkins, developed a now commonly used assay to study ALDH levels in individual cells.
Yet, scientists lacked an explanation for why post-transplant cyclophosphamide effectively curtailed acute and chronic GVHD.
Advertisement
Using polymerase chain reaction methods that amplify DNA and Jones' assay that detects by-products of ALDH, the Johns Hopkins team found that regulatory T-cells express high levels of ALDH.
"These regulatory T-cells are resistant to post-transplant cyclophosphamide and likely subdue the autoimmune-like response of the donor's bone marrow, preventing GVHD," says Christopher Kanakry, M.D., first author of the study and clinical fellow at the Johns Hopkins Kimmel Cancer Center. Patients receiving standard immunosuppressive drugs after transplant, as opposed to high-dose cyclophosphamide, have slower recovery of regulatory T-cells in their blood, adds Kanakry.
Advertisement
Luznik says his team is continuing to study methods to improve post-transplant cyclophosphamide, and it may be possible to use these findings to add other relapse-fighting therapies early after transplant. "Our findings may also lead to even wider acceptance of post-transplant cyclophosphamide," he said.
Funding for the study was provided by the National Institutes of Health, National Cancer Institute and National Heart, Lung, and Blood Institute (HL110907, CA122779, CA15396, UL1-RRO25005, and HL007525), the Conquer Cancer Foundation of the American Society of Clinical Oncology and Otsuka Pharmaceutical.
The assay (Aldefluor) used in this research was developed and patented by Richard Jones. Under a licensing agreement between Aldagen and the Johns Hopkins University, Jones is entitled to a share of royalties received by the University. The terms of this arrangement are managed by Johns Hopkins University in accordance with its conflict-of-interest policies.
In addition to Luznik, Kanakry and Jones, scientists contributing to the research include Sudipto Ganguly, Marianna Zahurak, Javier Bolaños-Meade, Christopher Thoburn, Brandy Perkins, Ephraim Fuchs and Allan Hess.
Source-Newswise