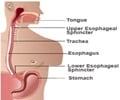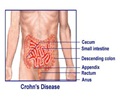
Previous research has linked a shortage of glutamine in the gut with the seepage of toxins and bacteria through the intestinal wall, irritating nerves and creating disease symptoms.
Scientists said that trying to generate glutamine in the disordered bowel by silencing this RNA segment could open up a whole new way of thinking about treating the diarrhea-predominant type of irritable bowel syndrome (IBS).
This form of the disorder is characterized by diarrhea and bloating as well as chronic abdominal pain that is difficult to treat.
About a third of IBS patients have the diarrhea-predominant type, another third experience consistent constipation, and the rest experience alternating bouts of diarrhea and constipation.
"We treat the disorder, but we still don't understand it completely. We often have to use multiple therapies to attack the symptoms, but the pain is by far the most difficult to treat. For some patients, the pain responds only to escalating doses of narcotics or tricyclic antidepressants," said scientists.
Advertisement
Lower levels of glutamine were seen only in tissue samples from patients with the diarrhea-predominant type of IBS.
Advertisement
The resulting irritation to nerves in the colon is believed to contribute to diarrhea and abdominal pain.
The finding suggests that the glutamine deficiency is connected to the increased intestinal permeability, which dramatically increases the likelihood that diarrhea-predominant IBS symptoms will follow.
"We've known about characteristics of this disease, but we didn't know the reasons behind them. This study helps us connect everything together. Maybe if we can modulate the microRNA, we can heal the disease. That is our whole hypothesis," said QiQi Zhou, assistant professor of internal medicine at Ohio State and lead author of the study.
The research was published in a recent issue of the journal Gut.
Source-ANI