Excessive and rapid weight loss after undergoing minimally invasive surgical treatment of morbid obesity may increase the risk of internal hernia, surgeons have warned.
(Internal hernia is a defect in the abdominal cavity that allows abdominal structures, such as the intestines, to move out of their natural position. However, the condition can be corrected surgically before it leads to potentially serious bowel obstruction.)Based on findings from a study presented at the 2008 Clinical Congress of the American College of Surgeons, the surgeons are encouraging physicians who see patients after bariatric surgery to evaluate or refer those who have lost more weight than expected for a surgical consultation if they also have intermittent or persistent abdominal pain. “Surgeons who perform this kind of procedure should be aware that patients who are rapidly losing weight may be at higher risk for internal hernia, and they should monitor them for signs of the condition. This is also the case for general surgeons who see patients in an emergency department. It’s our job to educate general surgeons who see patients who have abdominal pain and have lost a tremendous amount of weight in a quicker than expected period of time to be on the lookout for internal hernia as a possible cause of the symptoms,” according to Eric S. Bour, MD, FACS, Greenville Hospital System, University Medical Group–Bariatric and Minimal Access Surgery and Bariatric Medical Director of Hillcrest Memorial Hospital, Simpsonville, SC.
The surgical group also is counseling patients who have lost an excessive amount of weight in a short period of time after a bariatric operation to consult a surgeon if they have suspicious symptoms. “We caution patients if they start to develop episodes of abdominal pain or bilious vomiting that they should consult their surgeon and go through a workup,” Dr. Bour said.
The study is the first to focus specifically on a possible link between rapid and excessive weight loss and internal hernia. The study included 786 patients who underwent a laparoscopic gastric bypass operation between 2002 and 2007. A total of 24 patients in this population developed internal hernia, and 19 of them had periods of weight loss more than 125 percent greater than expected at one or more time points after the operation. Patients who have had gastric bypass are expected to lose 40 percent of their excess weight by three months after the surgical procedure, 60 percent by six months, 75 percent by nine months, and 85 percent by 12 months. A gastric bypass operation reduces the size of the stomach and redirects food past the small intestine to the large intestine.
Dr. Bour and his colleagues explored the relationship between rapid and excessive weight loss and internal hernia because the condition often remains hidden and there is currently no clear way of predicting which patients may develop it. Internal hernia affects between four and 10 percent of patients who have had a laparoscopic gastric bypass procedure, he said.
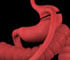
Internal hernia occurs when the bowel slips or herniates through an opening that was created in the mesentery (tissue that contains the blood supply and lymphatic drainage of the bowel) during the gastric bypass operation. The procedure divides the small bowel into parts. One is surgically moved into the upper part of the abdomen and connected to a newly formed and smaller stomach pouch, and the other part is connected to the small intestine downstream.
Advertisement
Internal hernia is corrected by surgically returning the herniated portion of the bowel to its proper position and closing defects with sutures to prevent serious complications, such as strangulation of the small bowel and incarceration or trapping of a segment of bowel within the hernia.
Advertisement
Source-Newswise
RAS/SK