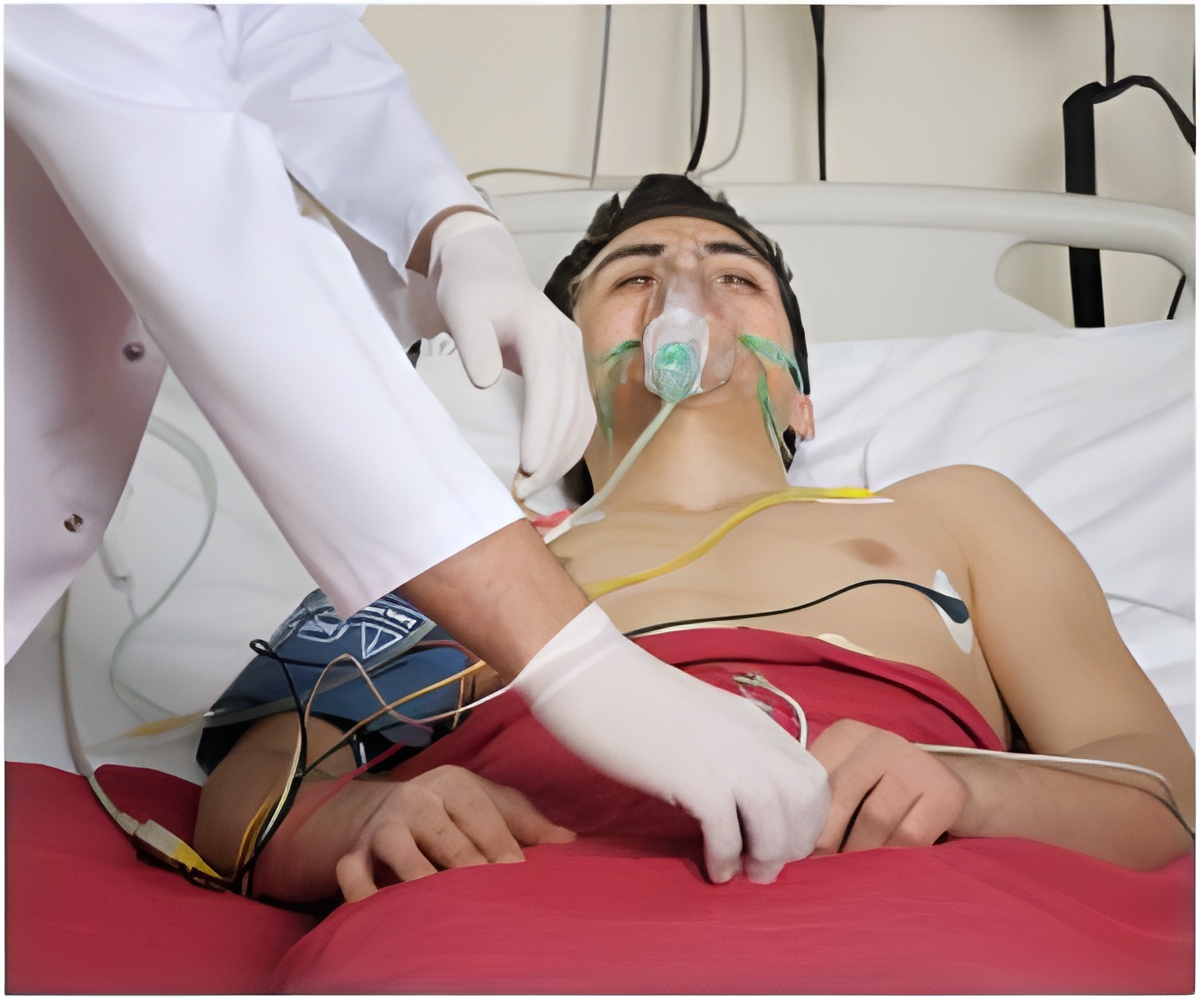
‘Emergency treatment for seizures begin with management of the airway, breathing and circulation, followed by medication interventions and rapid escalation of therapy to stop the seizures and prevent complications.’
Tweet it Now
Seizures may be convulsive with jerking rhythmic movements of the arms and/or legs, or they may be non-convulsive, with seizure activity indicated through more subtle signs. "A seizure can quickly change from a stressful situation to a life-threatening emergency. Without rapid assessment and treatment, seizures that progress to status epilepticus can cause permanent damage," said co-author Thomas Lawson, an acute care nurse practitioner in the neuroscience critical care unit at The Ohio State University Wexner Medical Center, Columbus.
Using recently updated guidelines for the evaluation and management of status epilepticus from the Neurocritical Care Society, the article provides specific nursing considerations related to caring for patients during this emergency.
"With their role at the patient's bedside, nurses are uniquely positioned to assist with the identification and management of status epilepticus to minimize long-term complications," Lawson said.
The article outlines priorities for nursing care, from the initial five minutes, through the first 15-minute and 60-minute windows, to the following 12 to 24 hours.
Advertisement
Once seizures are diagnosed, emergent treatment begins with management of the airway, breathing and circulation, followed by medication interventions and rapid escalation of therapy to stop the seizures and prevent complications.
Advertisement
The article addresses other nursing-specific considerations related to patients who are experiencing status epilepticus, such as gastrointestinal, dermatologic and neurologic concerns.
Source-Newswise