‘Huperzine A inhibits the enzyme acetylcholinesterase, and can increase the levels of acetylcholine in the brain which prevents seizures.’
Tweet it Now
Huperzine A comes from the club moss Huperzia serrata and has been used in traditional Chinese medicine. The compound has been tested for the treatment of inflammation and neurological disorders, including Alzheimer's disease and schizophrenia. Children with Dravet syndrome experience early-life seizures due to high fever as well as other types of seizures and developmental delays. Although the condition can be controlled with some antiepileptic drugs, most patients do not achieve adequate seizure control.
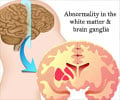
Most cases of Dravet syndrome are caused by "de novo" (not inherited) mutations in a sodium channel gene called SCN1A. The channel allows sodium to quickly enter into the cell, and forms part of the molecular machinery that is critical for how an electrical signal forms and travels along a neuron.
In Dravet syndrome, the mutations often inactivate the gene, while SCN1A mutations in GEFS+ change properties of the sodium channel without inactivating it completely. Both types of mutations lead to increased neuron excitability.
"We think that huperzine A could normalize the balance between neuronal inhibition and excitation in patients with SCN1A mutations, thereby protecting against seizure generation," says senior author Andrew Escayg, PhD, associate professor of human genetics at Emory University School of Medicine.
Advertisement
SCN1A mutant mice exhibit increased susceptibility to seizures induced by hyperthermia, which serves as a model of human febrile seizures. In the Frontiers paper, almost all SCN1A mutant mice exhibited a seizure when their core body temperature reached 40°C.
Advertisement
In these experiments, the scientists observed that the protective effect against electricity-induced seizures in normal mice diminishes after 12 days of daily huperzine A administration, but "complete protection" is maintained in the SCN1A-mutant mice.
"The protection observed in normal mice suggest huperzine A might also increase seizure resistance in other forms of treatment-resistant epilepsy. While these results are encouraging, further research will be required to determine suitability of using huperzine A as a clinical treatment for epilepsy," Escayg says.
In mice, the scientists observed some transient side effects from huperzine A administration: hypothermia, muscle twitching and lethargy. However, they determined that hypothermia does not contribute to seizure protection. Previous clinical studies have reported side effects such as nausea and vomiting. Wong and Escayg are now testing whether huperzine A can reduce the frequency of spontaneous seizures in their mouse models.
Source-Eurekalert