The process of how 2014 to 2017 physician-researchers at the 2019 Pediatric Academic Societies Meeting in Baltimore made their NICU a center of excellence for increasing the admission body temperature of their very low birth weight babies to greater //than 36 degrees has been explained.
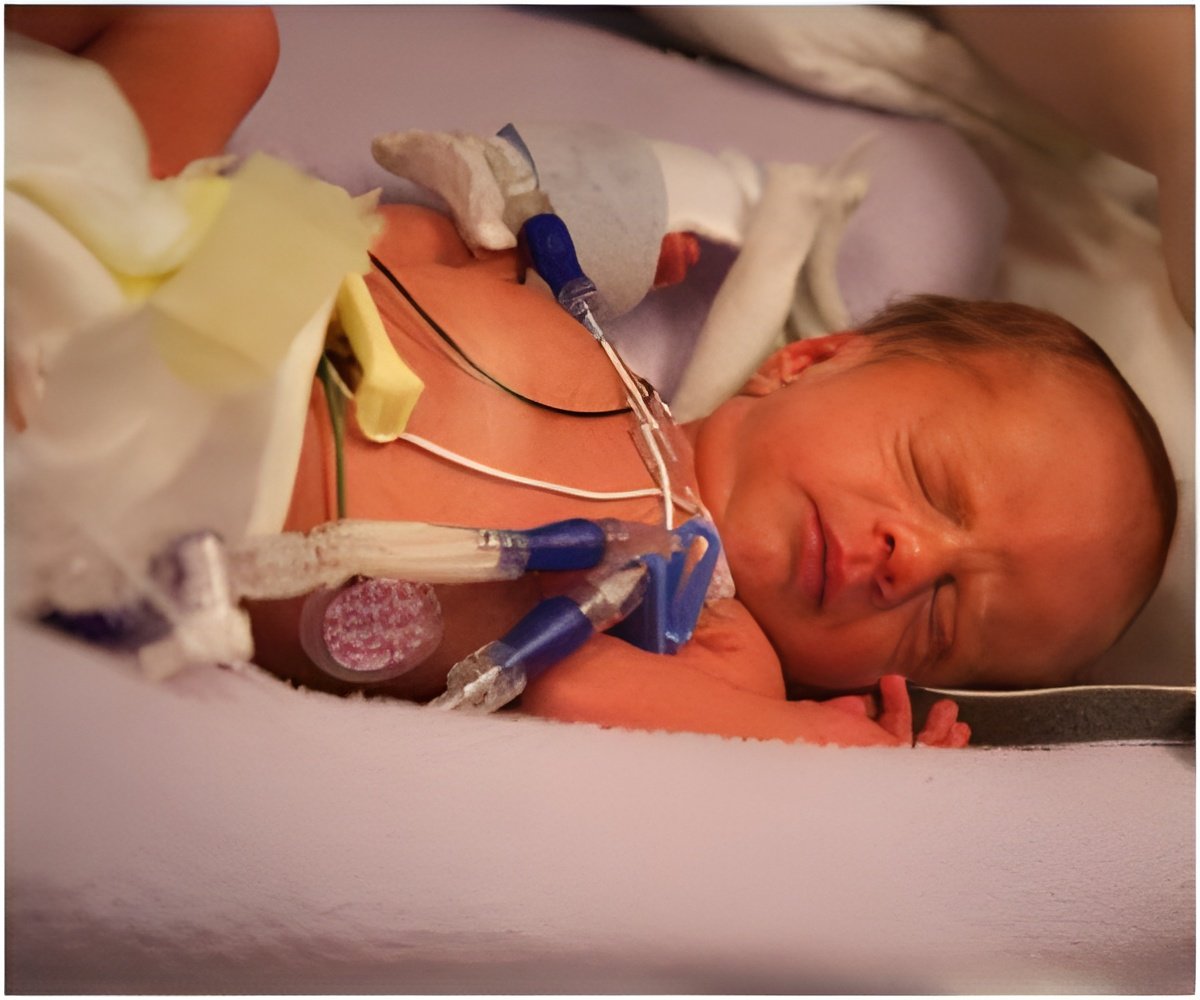
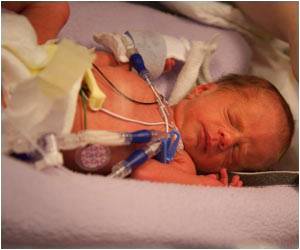
In several years preceding 2014, the medical staff of the Neonatal Intensive Care Unit (NICU) at University Hospitals Rainbow Babies & Children's Hospital and UH MacDonald Women's Hospital in Cleveland faced the problem of having almost 24 percent of VLBW (Very Low Birth Weight <1500 gms) babies of having a temperature of less than 36 degrees at the time of NICU admission. VLBW neonates are vulnerable to cold stress, which is associated with increased morbidity and mortality. Temperatures less than 36 degrees C are defined as hypothermic for these fragile babies by the World Health Organization. UH began quality improvement initiatives in 2014 to improve the temperatures.
Four thousand babies are delivered annually at UH MacDonald Women's Hospital; 150 of them VLBW neonates. VLBW babies are transferred to the 82-bed Level IV NICU next door in UH Rainbow Babies & Children's Hospital.
The team's goal was to decrease the rate of NICU admission hypothermia for all inborn VLBW neonates from 24 percent to less than five percent in five years.
They met their goal through a model for improvement quality initiative, through a comprehensive Key Driver Diagram (KDD) and several cycles of Plan-Do-Study-Act (PDSAs). For example, they minimized heat loss in the delivery room, during resuscitation and transfer to the NICU, among other measures.
Their results: 97.5 percent reduction of hypothermia (temperature less than 36 degrees) over a period of four years, from 24 percent to 0.6 percent in the VLBW babies. Ongoing work continues at the hospitals to sustain these measures.
Source-Eurekalert