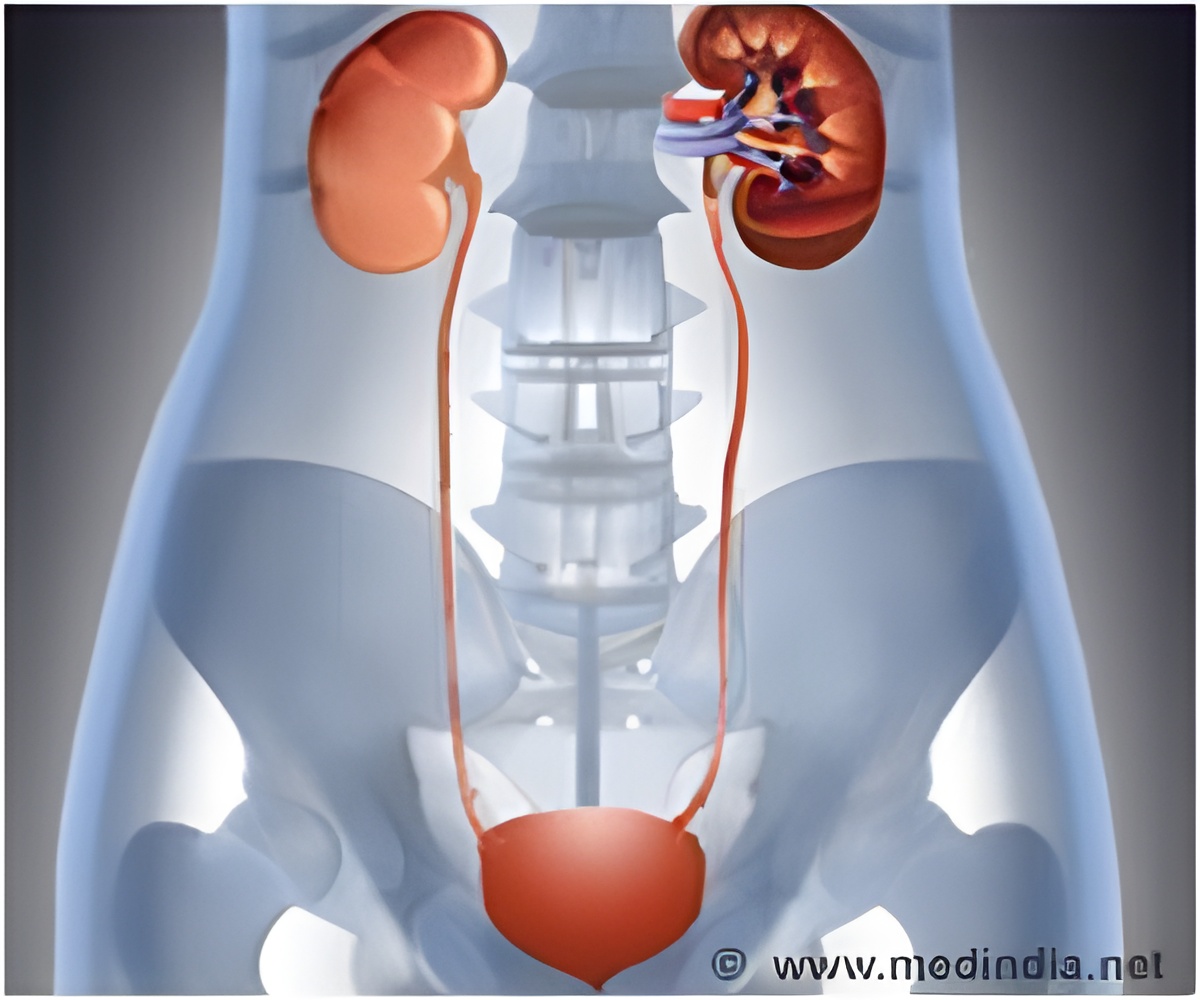
What Factors Affect Toxic Effects of HES on Kidney Cells? Hydroxyethyl starch is a starch derivative that has been widely used for fluid resuscitation with volume expansion for critically ill or injured patients in shock. A growing body of evidence suggests that HES solutions may have harmful effects, including an increased risk of kidney injury and death.
In previous studies, Dr Wunder and colleagues found that HES caused impaired kidney function in animals with sepsis (severe infection). Those studies showed that HES was localized mainly in the kidney PTCs. The researchers performed a series of in-depth follow-up experiments to look at factors influencing the toxic effects of HES on cultured human PTCs.
Most of the factors assessed had no major influence on reductions in cell viability caused by HES. Cellular toxicity was unrelated to the type of "carrier" solution used in the cell cultures, the use of HES made from different origins (potato versus corn starch), or the time cells spent in culture with HES.
The toxic effects were also similar for HES solutions of different molecular weights. That's an important finding, as newer low-molecular weight HES solutions were thought to be safer than previous products. There was also no evidence that the toxic effects of HES were related to the presence of inflammation.
Instead, the only significant factor was the total mass of HES molecules. The effect was dose-dependent: the greater the molecular mass, the greater the evidence of cell toxicity. The toxic effects started very soon after PTCs were exposed to HEC, and further increased at higher doses.
Advertisement
The new study suggests that the molecular mass of HES is the major factor responsible for damage to kidney cells. Other factors have no significant influence—even with new low-molecular weight HES solutions, cellular-level toxic effects appear just as likely, once the total mass of HES molecules is taken into account.
Advertisement
Source-Eurekalert