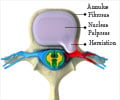
No Difference in Outcomes for Assigned Treatment The researchers analyzed data from the Spine Patient Outcomes Research Trial (SPORT), one of the largest clinical trials of surgery for spinal disorders. In SPORT, patients meeting strict criteria for herniated discs in the lumbar spine underwent surgery or nonsurgical treatment such as physical therapy, exercise, and pain-relieving medications. Patients with herniated discs experience back pain, leg pain (sciatica), and other symptoms caused by pressure on the spinal nerve roots.
The current analysis included eight-year follow-up data on 1,244 patients treated at 13 spine clinics across the United States. About 500 patients were randomly assigned to surgery (a procedure called discectomy) or nonsurgical treatment, although patients were allowed to "cross over" to the other treatment.
For the remaining patients, decisions as to surgery or nonsurgical treatment were left up to the patients and their doctors. Standard measures of pain, physical functioning, and disability were compared between groups.
Consistent with previous data from SPORT, patients assigned to surgery tended to have better outcomes. However, because many patients did not actually undergo their assigned treatment, the differences based on "intention to treat" were not statistically significant.
But Better Outcomes with Surgery, Based on Actual Treatment When outcomes were compared for patients who actually underwent surgery versus nonsurgical treatment, significant differences emerged. On a 100-point pain scale, pain scores averaged about 11 points lower in the surgery group. Measures of physical functioning and disability showed similar differences.
Advertisement
While average outcome scores were better with surgery, many patients had significant improvement with nonsurgical treatment. After eight years, about one-third of patients who were clinically indicated for surgery have chosen not to have operative treatment.
Advertisement
Lumbar disc surgery is one of the most commonly performed operations in the United States, although rates vary considerably in different regions. Past studies have suggested that surgery provides faster pain relief and recovery for patients with herniated discs, compared to nonsurgical treatment. However, it has been difficult to determine the true effects of surgery especially because of the high number of patients who cross over from nonsurgical treatment to surgery. This tends to underestimate the true benefits of surgery.
The long-term follow-up results from SPORT show that, for patients with confirmed herniated lumbar discs, "[S]urgery was superior to non-operative treatment in relieving symptoms and improving function." Dr Lurie and coauthors note that the peak benefits are achieved within six months after surgery and persist through eight years.
However, many patients treated without surgery "also showed substantial improvements over time," the researchers write. They add that patients who crossed over to surgery were more likely to be dissatisfied with their symptoms, felt like their symptoms were getting worse, and had initially worse physical function and disability.
Source-Eurekalert