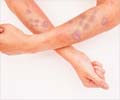
‘Discomfort in conventional health care settings and lack of HCV-related knowledge to fear of stigmatization that can result from an HCV diagnosis prevent patients with HCV from receiving the diagnoses and care.’
Tweet it Now
Talal, a leading expert in liver disease, said that a combination of factors all work to prevent these patients from receiving the diagnoses and care they need. Such factors range from discomfort in conventional health care settings and lack of HCV-related knowledge to fear of stigmatization that can result from an HCV diagnosis. That's in addition to insurance barriers and physicians' general reluctance to treat this population. According to the editorial, "New approaches for persons with substance use disorders are required at every step in the HCV care paradigm." The reason is that following a decade of fairly steady declines in this population, there have been recent sharp increases in HCV.
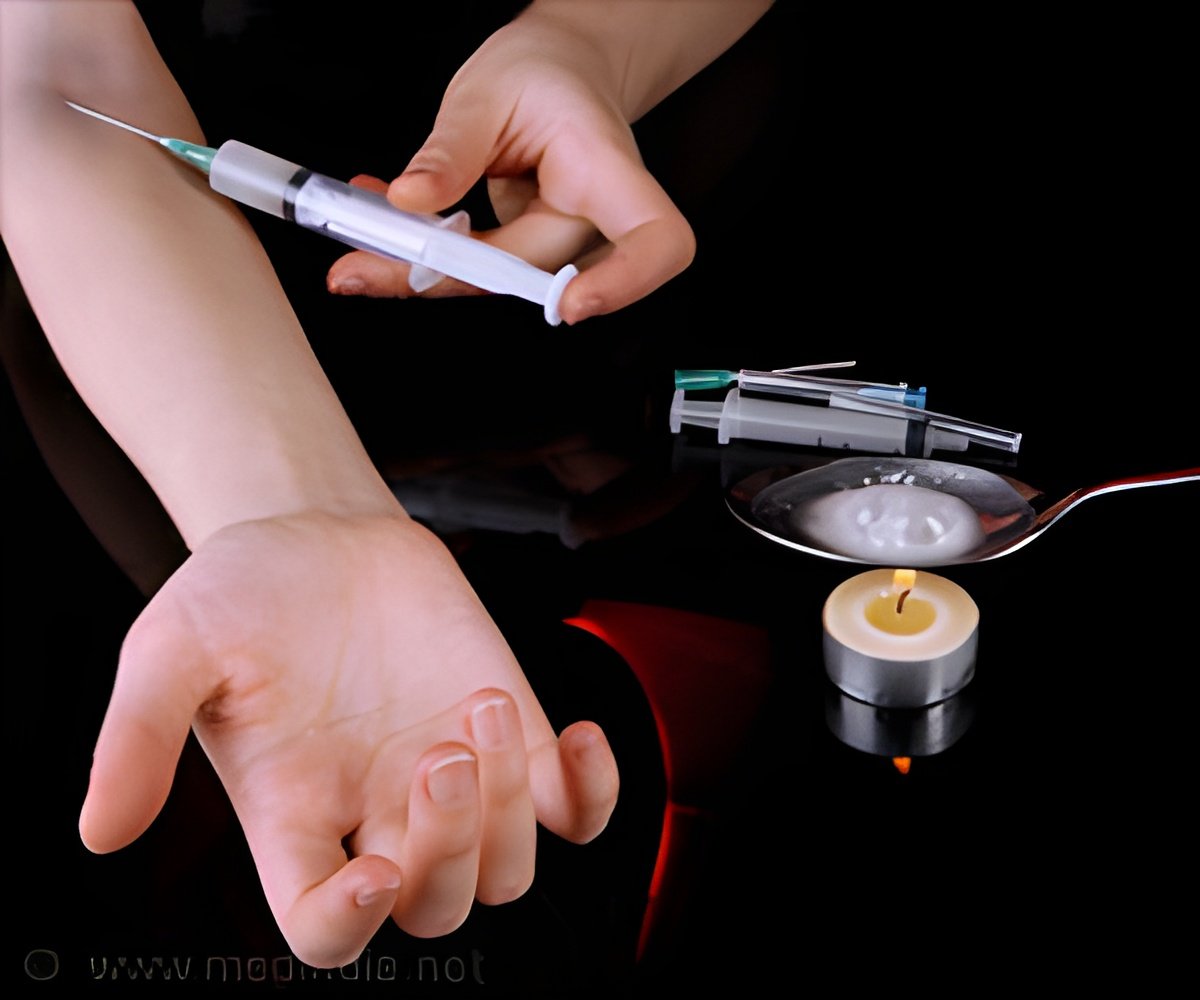
"We're seeing infection hotspots," Talal said, noting that this is partly a result of the opioid epidemic, particularly where needle exchange programs, for example, are not available. Such programs are key, Talal said, people who inject drugs account for approximately 75 percent of all new HCV infections.
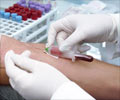
To better reach persons with substance use disorders, the editorial states, HCV screening and linkage to care must improve. Screening can be especially problematic because it typically requires two steps: confirmation that the person has been exposed to HCV through an antibody test followed by additional blood work to determine if the infection is active.
Currently, the second step must be conducted in a conventional laboratory, a setting these patients rarely access. Recent advances, however, are designed to assess whether all of required analyses could be done onsite.
Advertisement
Source-Eurekalert