Highlights
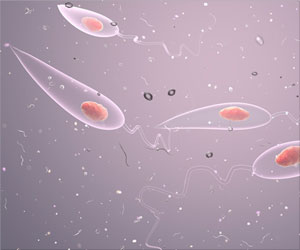
- Leishmaniasis is a parasitic disease transmitted by the bite of a sand fly.
- Scientists find new therapeutic targets for treating leishmaniasis.
T cells present in the immune system may trigger the activation of the signaling pathway which may lead to chronic inflammation. By blocking either of the two major pathway in the drugs may reduce lesions in animal models.
Phillip Scott, senior author, vice dean for research and academic resources at Penn Vet, said, "This is a neglected tropical disease, so it can be difficult to get the investment needed to develop new therapies."
"Our discoveries implicate the use of drugs in leishmaniasis that are already in use for other inflammatory diseases. This will be the foundation for clinical trials moving forward."
This work on leishmania in Brazil dates back 30 years. The skin damage may mainly occur to the direct effects of the Leishmania parasite when compared to an immune response. The CD8 T cells may protect the body from infections and promote increased disease.
"Here we discover the pathway by which they cause inflammation."
Testing IL-1 Protein For Tissue Damage
The IL-1 protein was found to be responsible for tissue damage. This was tested on infected animals that lack mature T cells to which CD-8 T cells were added back. The research team found high levels of IL-1 when compared to the infected mice which lack T cells.
The mice with CD-8 T cells when added with an inhibitor of IL-1 can greatly reduce the severity of the disease. Treatment with an inhibitor of a related molecule called IL-1 is not nearly as effective.
Anakinra drug that blocks the IL-1 receptor may help to treat rheumatoid arthritis. This may reduce the skin pathology in mice.
The authors also found Scott, Novais and colleagues, found that IL-1 need to be processed by an enzyme to become active if this can be a potential therapeutic target.
Caspase enzymes is one of the type of enzymes that can be processed by IL-1, These are implicated as requisite for the CD8-induced pathology in leishmaniasis.
NLRP3 inflammasome is a protein complex which is responsible for processing caspase-1 and may be required to develop leishmania-related skin lesions.
The two inhibitors of NLRP3 inflammasome is being tested. One of which is an approved diabetes drug glyburide, which prevents the mice from developing severe disease.
These findings were assessed in humans by carrying out skin biopsies from leishmaniasis patients. The lesion biopsies in culture was found to produce more IL-1 when compared to normal cells. And also treating the lesion biopsy may reduce the amount of IL-1 culture cells that were released.
The author concluded that there is solid evidence in the mouse which depicts that blocking the pathway with drugs may block pathology, but may or may not clear the pathology in patients.
Further clinical trials are carried out to test the efficacy of drugs like anakinra or glyburide.
References
- Fernanda O. Novais et al, CD8+ T cell cytotoxicity mediates pathology in the skin by inflammasome activation and IL-1β production, PLOS Pathogens (2017);DOI: 10.1371/journal.ppat.1006196
Source-Medindia