Highlights
- In U.S, the most common cause of liver transplants in children was found to be biliary atresia
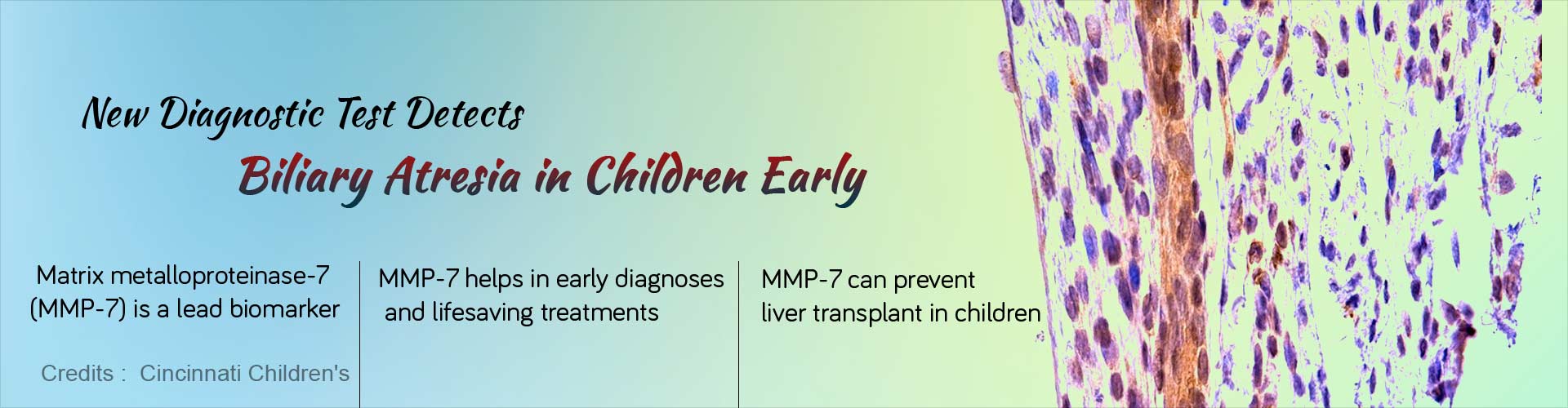
- A lead biomarker called Matrix metalloproteinase-7 (MMP-7) aids in early diagnoses and lifesaving treatments
- Early diagnosis and prompt surgical intervention could be the best predictors for a successful treatment
Molecular markers of the disease have been identified in blood samples that can accurately diagnose the condition with 90 percent sensitivity and specificity in infants, explained Jorge Bezerra, MD, the lead investigator, and director of Gastroenterology, Hepatology, and Nutrition.
The research team was led by Cincinnati Children’s Hospital Medical Center.
"From a broad screen of over 1,000 proteins, we found a unique protein associated with biliary atresia. Testing this protein as a diagnostic biomarker in two additional groups of babies to validate accuracy, it passed with flying colors," he said.
He also said that these findings were found to have real implications in diagnosing and caring for these babies.
A liquid called bile is produced by the liver cells that helps digest fat and also carries waste products from the liver to the intestines.
The research team suggests that early diagnosis and prompt surgical intervention could be the best predictors for a successful treatment. However, the current diagnostic methods available are time-consuming and imprecise.
Biliary atresia also has several causes including viruses, environmental toxins and a dysregulated immune system, which makes it more challenging to identify a faster, more effective and less invasive diagnostic methods.
Bezerra and his colleagues, including first author Chatmanee Lertudomphonwanit, MD, of Cincinnati Children’s and Ramathibodi Hospital (Mahidol University) in Bangkok of Thailand said that it is a high priority to identify better diagnostics for early medical interventions.
Blood Proteomics
The blood of 70 patients with biliary atresia was analyzed to look for molecules and to identify proteins that have increased when the disease is progressing.
The research team performed a large-scale proteomics analysis of about 1,000 proteins and their levels in the blood.
Matrix metalloproteinase-7 (MMP-7) was the lead biomarker that the research team has identified. MMP-7 is an enzyme that breaks down tissues and is associated with several disease processes.
While testing the diagnostic effectiveness of MMP-7, the research team found that there were about 97 percent sensitivity and nearly percent specificity for biliary atresia.
Combining the currently available blood test with MMP-7, gamma-glutamyl transpeptidase (GGT) had increased the diagnostic accuracy and reduced the risk of misdiagnosing before the surgical intervention.
Proof-of-principal tests were performed in mouse models of the disease by the research team to examine the role of MMP-7 in the onset of biliary injury.
The results showed that MMP-7 is released during bile duct injury to promote obstruction and subsequent problems.
The research team further studied to see if MMP-7 damages bile duct tissues, where a pharmacologic inhibitor of the protein called as Batimastat was used. This protein is approved only for laboratory research. Inhibiting this protein suppressed the onset of biliary atresia and also reduced tissue injury in mouse models.
Next Steps
Further research is required to validate in new population and also in the development of an assay that allows MMP-7 to be quantified, which can be used in the clinic as a readily available test for early diagnosis.
Bezerra will also be designing strategies to measure MMP-7 as a monitor of liver disease. He said, "It would be "intriguing" to determine whether Batimastat’s success in suppressing the disease in mice points to future treatments to target pathways linked to the enzyme."
What is Biliary Atresia?
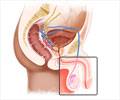
Biliary atresia is a congenital or acquired defect in the biliary transport system that occurs at birth or in a few weeks after birth. Bile produced by the liver is carried via ducts to the intestine to help in the digestion of fats.
The ducts present in the liver are called intra-hepatic ducts and the ones present outside the liver are called extra-hepatic ducts.
Biliary atresia is characterized by the absence of extra-hepatic ducts. This leads to failure in transport of bile presenting as jaundice. The bile then accumulates in the liver thereby damaging the liver cells due to inflammation and portal hypertension.
The liver undergoes scarring and fibrosis due to the stasis of bile and shrinks with time. This irreversible shrinking is called cirrhosis and can be life-threatening. The child needs a liver transplantation in due course to survive.
Reference
-
Biliary Atresia
- (https://www.cincinnatichildrens.org/health/b/biliary)
Source-Medindia