Women with knee osteoarthritis have more pain and poorer function than men, but similar physical activity prior to total knee replacement, according to an Iowa study published in the journal, Biology of Sex Differences.
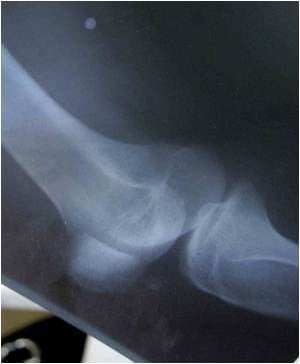
Osteoarthritis (OA), a degenerative joint disease, is a complex condition affecting the cartilage as well as other elements of the joint structure. The condition is associated with joint pain and disability. When osteoarthritis becomes severe, total knee replacement (TKR) is done to improve pain and function of the affected joint.Prior to TKR, women generally report higher pain intensity at rest and greater perceived functional deficits than men. They also perform worse than men on function measures such as the 6-minute walk and other tests. However, differences in pain sensitivity, pain during function, psychosocial variables, and physical activity levels in late stage osteoarthritis have still not been successfully determined.
Therefore, Shalome Tonelli and colleagues from the University of Iowa, USA, undertook a study to examine the differences in pain, pain sensitivity, function, psychosocial variables, and physical activity between women and men with knee osteoarthritis immediately prior to total knee replacement.
A total of 138 women and 70 men with knee osteoarthritis immediately prior (1 week) to total knee replacement surgery were selected for the study. Information regarding gender, age, race, marital status, education, income, duration of knee pain, OA grade (Kellgren-Lawrence), pain or OA in the contralateral knee, height and weight, and analgesia intake was collected. Assessment included the following:
• Pain was assessed using self-report measures (Brief Pain Inventory (BPI), Knee Injury and Osteoarthritis Outcome Score (KOOS), Short-Form 36 (SF-36)) and with a 0 to 20 numerical rating scale (NRS) at rest and during function tests.
• Pain sensitivity was assessed using quantitative sensory measures, including pressure pain thresholds, heat pain thresholds, and heat tolerance.
• Function was assessed with self-report measures (KOOS, SF-36), specific function tasks (timed walk, maximal active flexion and extension).
Results clearly showed a gender difference.
• Women had significantly higher pain intensity (7.34 ± 5.69) than men (5.69 ± 4.95) during the gait speed test as well as during active knee extension (women 8.40 ± 6.43 and men 5.93 ± 5.44). However, pain at rest did not vary significantly between women and men with the average resting pain measuring 3.77 ± 4.37 and 2.67 ± 3.81, respectively.
• Although women had significantly worse pain and more impaired function than men, their actual physical activity levels (accelerometry) did not significantly differ and their OA grade was significantly lower, that is, less severe.
• Women had more deficits on self-reported function on the SF-36 PF subscale and KOOS ADL subscale when compared to men, which means, women had reduced ability to perform the gait speed test and reduced knee active range of motion. The researchers think that the functional differences in knee OA subjects may in part be due to differences in quadriceps muscle strength between women and men.
• Regarding pressure pain thresholds, there was a greater mechanical pain sensitivity of the deep tissue in women when compared to men when a chronic pain condition such as OA is present.
• On the psychosocial level, scores were similar between women and men for depression, state anxiety, trait anxiety, pain catastrophizing, and perceived social support. Around 15 percent of both women and men screened positive for depression. Researchers think that depression explains a portion of physical activity levels in people with late-stage OA. Thus, ‘depression may be related to not only pain, but also function in people with OA’, they reason.
‘Our results clearly show that women have greater pain, greater pain sensitivity, and reduced function when compared to men. The role of sex needs to be further examined to determine if these pain differences are due to hormonal differences, socialization, or other factors’, concluded the authors. They further recommended that treatments should place a greater emphasis on pain management and improving function, particularly in women with osteoarthritis.
Source: Tonelli SM, Rakel BA, Cooper NA, Angstom WL, Sluka KA. Women with knee osteoarthritis have more pain and poorer function than men, but similar physical activity prior to total knee replacement. Biol Sex Differ. 2011 Nov 10;2:12.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3228720/
Source-Medindia