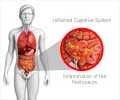
Peritonitis is inflammation of the membranes lining the abdominal wall and organs, caused by pathogens such as bacteria or other causes such as chemical exposure. Acute bacterial peritonitis (ABP) is a life threatening emergency that needs prompt medical treatment.
Peritonitis may be classified as primary/spontaneous peritonitis, secondary and tertiary peritonitis. In primary peritonitis, the infectious bacteria enter the peritoneal cavity through the circulatory or lymphatic system. Secondary peritonitis occurs due to infectious bacteria from a source within the peritoneum. Secondary infection is relatively common, taking the form of either generalized peritonitis or localized abscesses. Tertiary peritonitis is persistent or recurrent peritonitis that reappears at least 48 hours after the resolution of a primary or secondary peritonitis.ABP in patients with cirrhosis is considered to be due to bacterial translocation. Bacterial translocation is the process through which viable or non-viable bacteria and bacterial products (bacterial DNA or endotoxins) cross the intestinal lumen and come into the peritoneal cavity. This triggers an inflammatory process, which results in fluid shift into the peritoneal cavity. This accumulation of fluid coupled with decreased intestinal motility leads to abdominal distention.
The clinical presentation of ABP is highly variable. Presenting signs and symptoms can include fever, abdominal tenderness, nausea, or vomiting. Bacterial and endotoxin absorption into the bloodstream could lead to sepsis, affecting organ systems, and ultimately result in death. Hypoalbuminemia caused by protein loss and pulmonary complications like pneumonia may worsen the prognosis.
It is important to note that fluid displacement into the abdomen (known as third-spacing), could result in decreased blood volume or hypovolemia, which could further lead to low blood pressure and shock. Hypovolemia could lead to organ failure; therefore, rapid fluid resuscitation is very important in all patients with peritonitis so as to promote physiological stability. It should be noted that more aggressive restoration of intravascular volume should be provided to those with septic shock and organ failure.
Treating the cause and drainage of abscesses are the main desired outcomes in peritonitis. Secondary goals of treatment are elimination of infection and protection from adverse drug events as well as end-organ damage, including that to the lungs, liver, heart, and kidneys.
According to the Infectious Diseases Society of America (IDSA), it is recommended that antibiotics covering a wide range of organisms should be initiated within the first hour of the recognition of peritonitis in patients with compromised hemodynamic or organ function. It is important to consider the appropriate selection, dosing, and duration of antibiotics. For ABP, a 10- to 14-day course of antibiotics is recommended. A repeat peritoneal fluid analysis may be done to confirm effect of the treatment.
Traditionally, a combination of an aminoglycoside and ampicillin was used to treat ABP. Vancomycin is recommended when methicillin-resistant Staphylococcus aureus (MRSA) is the causative organism.
Patients should be evaluated after 48 hours to determine whether expanded antibiotic therapy is still warranted.
Acute renal failure is a vital predictor of death in spontaneous bacterial peritonitis (SBP) patients. Albumin has been used in SBP to cause plasma volume expansion to decrease the incidence of renal failure in patients with cirrhosis undergoing large-volume paracentesis. Prophylactic antibiotics (antibiotics used to prevent infection) should be administered to all patients who have had an episode of ABP and to patients admitted to a health center with gastrointestinal bleeding. Primary prophylaxis with fluoroquinolones in patients with a low ascitic fluid protein concentration is recommended.
Reference: Acute Bacterial Peritonitis in Adults; Michele Reed et al; US Pharmacist 2012.
Source-Medindia