Highlights
- The lesser developed countries face a disproportionate burden of cervical cancer.
- The American Society of Clinical Oncology (ASCO) has issued the first clinical practice guideline on human papillomavirus (HPV) vaccination based on global resource settings.
- The ASCO's guideline focuses on the use of HPV vaccination specifically for the prevention of cervical cancer.
The guideline includes recommendations according to four levels of resource settings-basic, limited, enhanced and maximal.
The levels include financial resources of a country or region and the development of its health system.
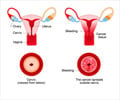
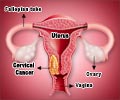
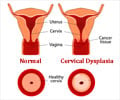
Cervical cancer is the fourth most common cancer among women worldwide. Lesser developed regions face a large and disproportionate burden of the disease.
In these regions including Africa and Latin America, about 85% of cervical cancer related diagnoses and 87% of cervical cancer deaths occur.
Vaccination Guidelines Based on Different Levels of Resource Settings Independent of the resources settings:
- two doses of HPV vaccine are recommended for girls ages 9 to 14 years, with an interval of at least 6 months and up to 12 to 15 months between doses
- girls who are HIV positive should receive three doses
- girls who are 15 years or older and have received their first dose before age 15, they may complete the two-dose series
- if they have not received the first dose before age 15, they should receive three doses
- vaccination may be given through age 26 years, in both cases
- girls who received one dose may receive additional doses between ages 15 and 26 years, if sufficient resources remain after vaccinating girls 9 to 14 years
- boys may be vaccinated in all settings, if there is at least a 50% coverage in priority female target population, sufficient resources, and such vaccination is cost effective
"Although HPV vaccine has been around for more than a decade, the uptake of the vaccine has been less than ideal in many places, including in high-resource countries such as the United States," said Silvina Arrossi, PhD, co-chair of the Expert Panel that developed the guideline and an official and researcher at the Instituto Nacional del Cancer in Buenos Aires, Argentina. "As an organization of cancer doctors, ASCO continues to endorse HPV vaccination programs and efforts to help spare more women around the world from this very difficult cancer."
The findings are published in the Journal of Global Oncology.
Reference
- Silvina Arrossi et al. Primary Prevention of Cervical Cancer: American Society of Clinical Oncology Resource-Stratified Guideline. Journal of Global Oncology; (2017) doi.org/10.1200/JGO.2016.008151
Source-Medindia