Highlights
- Hepatocellular cancer (HCC) is the second leading cause of death from cancer globally due to its poor prognosis and high frequency.
- Coffee is a complex mixture of //biologically active molecules, including caffeine, chlorogenic acid and diterpenes.These compounds possess antioxidant, anti-inflammatory, antifibrotic and anticarcinogenic properties.
- Drinking just one cup of coffee a day was associated with a 20 percent reduction in the risk of developing HCC.
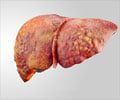
Hepatocellular carcinoma
Hepatocellular carcinoma (HCC) is the dominant histological subtype accounting for 85%–90% of cases.HCC most commonly develops in people with cirrhosis due to chronic viral hepatitis B (HBV) or hepatitis C (HCV), excess alcohol consumption, and/or non-alcoholic fatty liver disease. The incidence of liver cancer is increasing due to changes in these underlying risks and by 2030 the number of new cases will have been risen to 1.2million.
The findings showed that drinking just one cup of coffee a day was associated with a 20 percent reduction in the risk of developing HCC, two cups was associated with a 35 percent reduction, and up to five cups with a 50 percent reduction.
There was little data available above five cups a day to show what effect increasing consumption further may have. Lead author Dr Oliver Kennedy noted that “We’re not suggesting that everyone should start drinking five cups of coffee a day though. There needs to be more investigation into the potential harms of high coffee-caffeine intake, and there is evidence it should be avoided in certain groups such as pregnant women.”
It is a complex mixture of biologically active molecules, including caffeine, chlorogenic acid and diterpenes. These compounds possess antioxidant, anti-inflammatory, antifibrotic and anticarcinogenic properties, which may explain the observational data that coffee drinkers have lower rates of chronic liver disease (CLD), including fibrosis, cirrhosis and HCC.
Professor Peter Hayes of the University of Edinburgh, said, “We have shown that coffee reduces cirrhosis and also liver cancer in a dose-dependent manner. Coffee has also been reported to reduce the risk of death from many other causes. Our research adds to the evidence that, in moderation, coffee can be a wonderful natural medicine.”
Dr Kennedy also added, “Our findings are an important development given the increasing evidence of HCC globally and its poor prognosis.”
Increased coffee consumption has already been shown to protect against serious non-cancer chronic liver disease (cirrhosis), possibly due to the compound molecules in coffee possessing antioxidant, anti-inflammatory, anticarcinogenic, and other beneficial properties.
Reference
- Oliver John Kennedy et al., Coffee, including caffeinated and decaffeinated coffee, and the risk of hepatocellular carcinoma: a systematic review and dose–response meta-analysis, BMJ (2017) http://bmjopen.bmj.com/content/7/5/e013739.
Source-Medindia