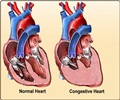
Highlights
- Treatment for congestive heart failure includes drug therapy and use of defibrillators.
- Exercise was strictly prohibited for patients with heart failure as it was thought to add strain to heart muscles and affect its pumping function.
- According to new recommendations, exercise training in heart failure does not deteriorate dilatation and function of the heart and seems to be safe.
Patients with this condition were strictly forbidden from engaging in physical training because of fear that this would further compromise the heart’s pumping function. Instead, they were mainly treated with drugs and by implanting defibrillators.
"Previously, congestive heart failure was primarily treated with drugs. The range of treatments was expanded by the use of cardiac pacemakers to optimize heart muscle contraction and the implantation of defibrillators intended to improve myocardial function and prevent sudden cardiac death due to arrhythmia", explained Professor Martin Halle, Professor of Preventive and Rehabilitative Sports Medicine at TU Munich.
But recent studies have proved that physical training is not harmful to the heart. On the other hand it can increase endurance of heart muscle and reduce re-hospitalization rate, which is the rate of re-hospitalization due to worsening of symptoms.
Study
"With this study, we are able to prove that exercise training does not deteriorate dilatation and function of the heart and seems to be safe", concluded Halle.
They were assigned to three groups and over 52 weeks, they underwent high intensity interval training (HIIT), moderate continuous training (MCT) and recommendation of regular exercise (RRE).
Initially, all three groups underwent supervised training for three months and in addition, they were given the recommendation to continue the intervention for another nine months.
Patients that participated in 12 weeks of regular supervised exercise had better effects than those who just got a recommendation to train on their own.
"We actually observed a decrease in the size of the left ventricle, and with it, an improvement in pumping function", said Professor Halle. "This increased their physical fitness."
No significant differences between interval training at high intensity and a standard therapy with continuous training at moderate intensity was detected.
"We actually observed that this training revealed the best improvements and that not exercising was significantly worse regarding pump function and hospitalization", said Professor Halle.
"Overall, this new study underscores how advisable regular physical training at moderate intensity is for patients with systolic heart failure", Halle concluded - "but I would rather discourage high intensity exercise until larger studies will prove this to be as safe."
The doctor also offered the following concrete tip- Moderate training means around one hundred steps per minute or 3,000 steps in 30 minutes.
The benefits of individualized exercise therapy for cardiac patients include
- decreased strain on the heart and improvement in function of the heart muscles
- improvement in dilation of blood vessels and lowering elevated blood pressure
- improved oxygen uptake for energy production, endurance and performance
- decreased risk of cardiac and vascular emergencies such as heart attack and stroke
Reference
- Martin Halle et al. High Intensity Interval Training in Heart Failure Patients with Reduced Ejection Fraction. Circulation; (2017) doi.org/10.1161/CIRCULATIONAHA.116.022924
Source-Medindia