World TB Day falls on March 24th, and this year’s theme aims at putting an end to the global epidemic and bring TB-related deaths to zero. Of the 9 million people who get sick with TB every year 3 million are missed i.e. they fail to get the care they need. The World TB Day 2014 targets to ‘reach the 3 million; find, treat and cure TB.’
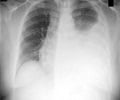
March 24 is observed globally every year as World TB Day; it was on the same date in 1882 that Dr Robert Koch astounded the world with his discovery that TB bacillus is the cause of tuberculosis. The announcement came at a time when TB was rampant in Europe and the Americas killing one out of every seven people affected.TB is a curable disease. It is a bacterial infection that can spread to any organ in the body though the lungs are most commonly affected. A six-month course of drugs can completely cure most people with TB. An incomplete treatment is more dangerous, it harbingers the return of TB in a more resistant form. In 2012, 8.6 million people fell ill with TB, around 1.3 million people died.
The global war against TB has saved nearly 22 million lives since 1995; a 45 % decrease in TB has been registered since 1990. Despite these reassuring statistics the rash truth that 3 million people are “missed” each year serve as a pointer to the inefficiency of our health systems. The proportion of missed cases has remained the same for the past seven years. Nearly two-third of the missed cases reside in South Asia and Africa.
Why are 3 million missed?
* People with TB may not access care at all- Awareness of TB appear to be limited. Those with TB continue to suffer discrimination, stigma, rejection and social isolation. The very poor who cannot afford user fees or transport may keep away from health care.
* Those who access health services may not get diagnosed- Overburdened and undertrained healthcare staff may fail to identify the symptoms; inaccurate and inappropriate tests can prevent a proper diagnosis. Children with TB are the ones often missed or overlooked. Children are estimated to account for half a million new TB cases every year and nearly 74000 deaths.
Reaching three million is an arduous task. We need an aggressive campaign to ensure access and coverage for all; TB ‘hotspots’ need to be recognised. The underserved and vulnerable communities need to be identified. Attempts must be made to reduce the stigma associated with TB. We need more investment in basic research. Fast diagnosis, treatment and prevention require the development of better tools- efficient screening tests, newer drugs and vaccines. We need to strengthen specimen transport and patient referral systems. Healthcare providers should be trained adequately.
The participation of female Health Extension Workers (HEWs) in Ethiopia, an area of over 3 million people, doubled TB case notification in years’ time. HEWs are lay workers with a small government salary who provide basic services to their community. They were trained to identify the symptoms of TB, collect sputum and prepare slides.
Better screening of people attending health facilities did wonders in Afghanistan. It trained staff across 47 health facilities in screening and sample collection; within a year, over 70 % more cases were identified than the year before.
Myanmar developed an evidence based national response planning to identify its heavy burden of missed TB patients. A national survey found out a higher burden in urban areas, in men, and among the elderly.
New molecular tests that can better identify cases of TB than smear microscopy have been developed. Xpert MTB/ RIF is such a rapid diagnostic test; countries such as Moldova and South Africa are working hard to improve access to this test.
Countries like India, Pakistan and the Philippines are trying hard to engage the private providers in their national programmes. China improved her surveillance systems by setting up a national web-based for mandatory reporting of infectious diseases. The use of a low cost system that involved the use of electronic score cards on mobile phones allowed health workers in Karachi, Pakistan to better identify childhood TB; the number of identified cases was six times more than what was done in previous years.
Examples of successful interventions do not end here; the cost of inaction is heavy. A case of TB can infect up to 10 people a year. Well, keeping all this in mind, let us all be part of the Stop TB Partnership, and play our roles in eliminating this evil.
Reference:
http://www.stoptb.org/events/world_tb_day/
Source: Medindia