- Scientists find that stem cells that develop into smooth muscle cells raise calcification in arteries.
- The stem cells develop into osteoblasts that are essentially bone cells.
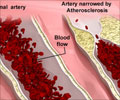
- This restricts the flow of blood and increases risk of atherosclerosis in chronic kidney patients.
- The study provides scope for better drug therapy to control atherosclerosis risk.
Vascular Calcification in Chronic Kidney Disease Patients
There are two types of calcification of the arteries that take place in chronic kidney disease patients.
A) Atherosclerotic calcification:
- This is present in the intimal layer
- Leads to atherosclerosis
- Causes cellular necrosis
- Deposition of lipids
- Inflammation
- Osteogenesis that includes induction of osteoblasts
- This type of calcification is found to be common in chronic kidney disease patients and people with diabetes.
- Occurs in the vascular smooth muscle cells.
- It is also known as Monckeberg Sclerosis.
Current studies are aimed at the association between vascular calcification and osteogenesis. In calcified medial arterial layers as well as in atherosclerotic plaques, there have been expression of key regulators of bone structural proteins.
Gli1 cells are adult stem cells that are present in the outer layer of the arteries. These stem cells have the ability to differentiate into a number of connective tissue like fat, bone and smooth muscle. The study by Dr. Benjamin Humphreys and colleagues has found that these stem cells are responsible for the mineral deposits that clog the arteries.
Gli1 cells are stem cells that are directed to generate smooth muscle cells in the arteries to enable healing and effective contractive ability of the arteries. In chronic kidney disease, this mechanism is disrupted with changes in signaling pattern resulting in these stem cells being converted into osteoblasts, which are a type of bone cells that increase the deposition of calcium in the arteries.
Dr Humphreys adds, "We expect to find osteoblasts in bone, not blood vessels. In the mice with chronic kidney disease, Gli1 cells end up resembling osteoblasts, secreting bone in the vessel wall. During kidney failure, blood pressure is high and toxins build up in the blood, promoting inflammation. These cells may be trying to perform their healing role in responding to injury signals, but the toxic, inflammatory environment somehow misguides them into the wrong cell type."
Tissue Studies:
The researchers from The University School of Medicine in St. Louis studied tissue samples of people who died from chronic kidney disease to understand the effects on the aorta. The scientists found that mineral deposits in the aorta of humans was found in the same place as those found in mice, suggesting the mice studies would be accurate in understanding the pathogenesis of this condition.
Mice Studies:
The researchers removed the adult stem cells Gli1 in mice and observed the deposition of calcium in their aorta. It was found that the there was no calcification of the aorta in mice.
Another study by researchers from Brigham and Women’s Hospital (BWH) ablated the Gli1 cells in mice with cardiac and kidney fibrosis, without harming any other cell. It was found that the there was a reduction in fibrosis with a rescue of the function of the heart.
Such studies point towards
- Gli1 being a possible target for drug therapy to lower calcification and to restore the functions of the organs.
- Cautious prescription of oral calcium for people on dialysis or with chronic kidney disease
- The Gli1 cells can be induced to produce smooth muscle cells which will aid in healing the blood vessels.
A considerable number of individuals with chronic kidney disease die of atheroscleroses which can be avoided by effective targeted treatment such as targeting the Gli1 cells. Stems cells have always held an enviable position in medical studies and with the right kind of stimulation, the Gli1 cells reverted as healers rather than sealers.
References:
- Vascular Calcification: The Killer of Patients with Chronic Kidney Disease - (http://jasn.asnjournals.org/content/20/7/1453.full)
- Vascular calcification in chronic kidney disease - (http://www.ncbi.nlm.nih.gov/pubmed/16502129)
- Researchers have identified the cells responsible for fibrosis, the buildup of scar tissue - (https://health-innovations.org/2014/12/02/researchers-have-identified-the-cells-responsible-for-fibrosis-the-buildup-of-scar-tissue/)
Source-Medindia