Highlights:
- A low-cost test can identify patients at high risk of requiring dialysis or transplant accurately
- This simple test helps in screening for excess protein in the urine
- Targeting and treating these patients could help save the healthcare spend toward dialysis and transplantation
Read More..
Acute Kidney Injury
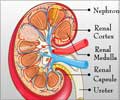
Acute Kidney Injury (AKI) is a condition where the kidneys are unable to filter waste from the blood unexpectedly. AKI can occur at any age due to various causes and has complex symptoms. More than 200,000 patients in the US and around 13.3 million globally are affected by AKI every year.Progression of kidney disease, kidney failure, heart disease, death and a greater likelihood of AKI recurrence are common in patients who recover.
Chronic kidney disease is diagnosed in around 20 percent of patients within three to five years.
Earlier studies have attributed an increase in hospitalization, costs from $5.4 billion to $24 billion to AKI. The costs for patients requiring dialysis with AKI were $11,016 to $42,077 higher, per hospitalization, than for those without AKI. An additional 3.2 days of hospitalization was required in the case of AKI. While the costs were higher than myocardial infarction and gastrointestinal bleeding, they were comparable to pneumonia, stroke and pancreatitis.
Proteinuria and AKI
Excess protein in the urine – Proteinuria, is a crucial indicator of kidney function that could indicate early kidney disease. An inexpensive, non-invasive test, proteinuria, though used by clinicians in other settings, is not commonly measured in patients after AKI occurrence.“There should be much more emphasis on the testing of proteinuria after AKI to identify high-risk patients,”said Chi-yuan Hsu, the lead author, Professor and Chief of Nephrology at UCSF. He added further, “This simple test carries important prognostic information not conveyed by serum creatinine.”
Emphasizing on the importance of measuring proteinuria Hsu said, “Too many providers rely on serum creatinine alone to assess the health of the kidneys, but they should not be falsely assured by the latter. Having a more complete picture of kidney health is necessary for proper clinical decision-making.”
Results of the Study
The findings of the study appear in JAMA Internal Medicine. About 1,538 hospitalized adults, equal numbers of those with and without AKI were studied in this decade long study. The research period was between December 2009 and February 2015, which included an annual in-person visit through November 2018 and semiannual phone contacts.In the average follow-up period of 4.7 years, kidney disease progression and end-stage renal disease were diagnosed in 138 patients overall (9 percent) and 58 patients respectively. Among patients with AKI, 97 (12.6 percent) had kidney disease progression.
A 1.5-times higher risk of disease progression was identified in patients with proteinuria after three months.
Improving Outcomes
One of the four North American clinical centers that participated in the study was Kaiser Permanente/UCSF. Hsu, who is the adjunct investigator at the Kaiser Permanente Division of Research also mentioned that in addition to getting tested, controlling blood pressure or taking medications to reduce proteinuria may also help lessen adverse outcomes.Hsu said, “Most patients with acute kidney injury are unaware of their condition, lack understanding of its natural history or predisposing factors, and desire more information. However, few discharge communications currently provided to these patients explain the condition or provide recommendations for care, which is needed throughout the care continuum.”
Reference:
- Simple test identifies patients at high risk for future dialysis or transplant - (https://www.ucsf.edu/news/2020/01/416506/simple-test-identifies-patients-high-risk-future-dialysis-or-transplant)
Source-Medindia