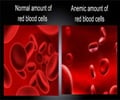
- STAT1 gene mutation leads to dysfunction of the immune system making the person susceptible to fungal, viral and certain bacterial infections.
- Current study conducted to assess response of patients to hematopoietic stem cell transplant (HSCT) for this condition indicates it is curative but associated with significant risks.
What is the Need to Assess Outcome of HSCT in STAT1 Gene Mutation
STAT1 gain of function mutation leads to an immunodeficiency/autoimmune like state with increased susceptibility to fungal infections such as Candida, viral infections including herpes simplex encephalitis and bacterial infections such as tuberculosis. The symptoms can range from mild to severe and life threatening. The condition was first described by Dr Okada in 2011.
It is believed that if hematopoietic stem cell transplant found to be safe and effective could offer the hope of a cure and relief from suffering for many of these patients.
Hematopoietic stem cell transplant has been tried in a few patients with severe disease and shown to be curative at least in one instance in published literature. However, the overall efficacy, safety and outcomes following HSCT in this condition have not been established.
Current study hopes to determine patient response to HSCT in a worldwide study across many centers taking into consideration factors such as donor engraftment, graft versus host disease, overall patient survival and other transplant related complications.
Response to HSCT In STAT1 Gene Mutation - Study Details
- The study involved 15 young patients, from nine different countries, with varying degree of complications caused by the STAT1 mutation.
- Patients were enrolled for the study through appeals to various transplant centers and consortia.
- The age of participants ranged from 13 months to 33 years.
- A diagnosis of STAT1 gain of function mutation was confirmed by the research team and established as the source of their illness.
- Centers across the world carried out treatment independently.
- Before HSCT was done, patients were administered chemotherapy to destroy the bone marrow which was the source of the disease causing STAT1 mutation.
- Following this, stem cell cultures obtained from healthy donors was transplanted into the patients in the hope of making the marrow healthy and disease free.
- The results were rather disappointing in that only 6 out of the 15 (40%) survived the HSCT; the only heartening factor was that 5 of these were completely cured and disease free at the end of the study.
- Over time the transplanted healthy cells decreased in number and the marrow went back to the pre-transplant state with the mutation. Subsequently the donor transplant was rejected.
- Strong and high dose chemotherapy to destroy diseased marrow also damaged host tissue causing failure of multiple organs including the immune system leading to severe life threatening infections.
- Younger patients fared better, probably because the cumulative effects of the disease, in particular infections might have been lesser.
- Only patients with severe symptoms should be considered for HSCT as the benefits may outweigh the risks
- Dose of chemotherapy needs to be reduced to decrease damage to host tissue, but diseased marrow has to be eradicated for the transplant to be successful. A fine balance has therefore to be maintained.
- Low dose chemotherapy may need to be supplemented with other treatments to neutralize host antibodies and prevent immune attack on donor stem cells and to prevent donor stem cell graft rejection.
- HSCT should be considered at an younger age itself since outcomes have been better.
References:
- Hematopoietic stem cell transplantation in patients with Gain of Function STAT1 Mutation - (http://www.jacionline.org/article/S0091-6749(17)30916-8/pdf)
- STAT1 gene - (https://ghr.nlm.nih.gov/gene/STAT1#conditions)