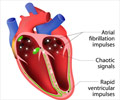
- In Atrial Fibrillation, the irregular beating of the heart predisposes the patient to a risk of clot formation and stroke.
- Anticoagulants thin down the blood and prevent clot formation, making them the drug of choice for reducing stroke risk in Atrial Fibrillation.
- Despite recommendations, aspirin is still preferred over anticoagulants in a significant number of these patients, according to a recent study.
They found out that in the first cohort of 210000 patients with a CHADS2 score (risk score signifying moderate to high risk for thrombosis) equal to or higher than 2, around 61.8% were treated with anticoagulants while the remaining 38.2% were prescribed aspirin alone. In the former group, 90.9% were prescribed warfarin.
The researchers even discovered that certain characteristics predicted the type of treatment received. Patients with a deranged lipid profile, coronary artery disease and history of MI or hypertension were more likely to be treated with aspirin while male patients and those with a history of stroke, systemic embolization, congestive heart failure and higher body mass index were given anticoagulants.
Similar findings were seen on analyzing the second cohort of 294642 patients with a CHA2DS2-VASC score (a score which includes more CHD risk factors) of 2 or more.
Aspirin Offers No Stroke Protection
Aspirin is an antiplatelet drug. It prevents platelets from clumping together and forming clots, but it does not act as a blood thinner like anticoagulants. Aspirin can definitely reduce clot formation in the arterial bed but does not offer protection against thrombosis in the heart.Sanjay Deshpande, MD and Samuel Wann, MD from Columbia St. Mary’s Hospital, Milwaukee wrote in their editorial titled ‘The Clot Thickens’ published along with the study that aspirin is ineffective for prevention of thromboembolism associated with atrial fibrillation while oral anticoagulants are far superior in the same. Moreover, aspirin is associated with a risk of bleeding, though small.
- AVERROES (Apixaban Versus Acetylsalicylic Acid to Prevent Stroke in Atrial Fibrillation Patients who have Failed or are Unsuitable for Vitamin K Antagonist Treatment) in 2010, and
- WOEST (What is the Optimal Antiplatelet and Anticoagulant Therapy in Patients with Oral Anticoagulation and Coronary Stenting) in 2013.
Need to Educate the Physicians
Editors Deshmukh and Wann noted that while American Heart Association still slightly supports aspirin use in patients with low risk of stroke but European Society of Cardiology and NICE in England do not recommend the use of aspirin to prevent stroke in patients with atrial fibrillation at all. Therefore, it was surprising to the researchers that even the most meticulous and talented cardiologists were prescribing aspirin alone in one-third of the patients.They speculated the reasons as under:
- Clinicians feel aspirin offers enough protection against stroke. It actually does not.
- The risk of bleeding associated with anticoagulants is a deterrent. The risk does exist but most of the times, the benefits outweigh the risk. Even aspirin is associated with a risk of bleeding.
- Patient non-compliance with regular intake of anticoagulants over a long period of time.
- Bias to follow conventional methods and resist change despite the evidence.
- Lack of awareness regarding the safer new anticoagulants that are associated with a lower risk of bleeding and offer better protection against thromboembolism.
- Resistance on the part of the patient to anticoagulants as the drugs are expensive, require following a regimen and are associated with some side effects.
- The abstractness of the benefit of stroke prevention which is hard to prove to a reluctant patient.
The authors therefore wrote, "Focusing on factors at the practices level, and not simply at the individual physician level, may prove important in future efforts to rectify proper prescription or (oral anticoagulation) in (A-fib) patients at risk for stroke."
References:
- Offer anticoagulants instead of
aspirin for stroke prevention
https://www.nice.org.uk/news/article/offer-anticoagulants-instead-of-aspirin-for-stroke-prevention - Aspirin Often Wrongly Prescribed for Atrial Fibrillation
https://www.nlm.nih.gov/medlineplus/news/fullstory_159459.html - Aspirin Instead of Oral Anticoagulant Prescription in Atrial Fibrillation Patients at Risk for Stroke
http://content.onlinejacc.org/article.aspx?articleID=2529509