Laid out, the gut lining would cover the area of a football pitch.
It must let nutrients from our foods through, but prevent invasion by disease-causing bacteria, at the same time hosting the trillions of beneficial bacteria needed for proper digestion and immune function.
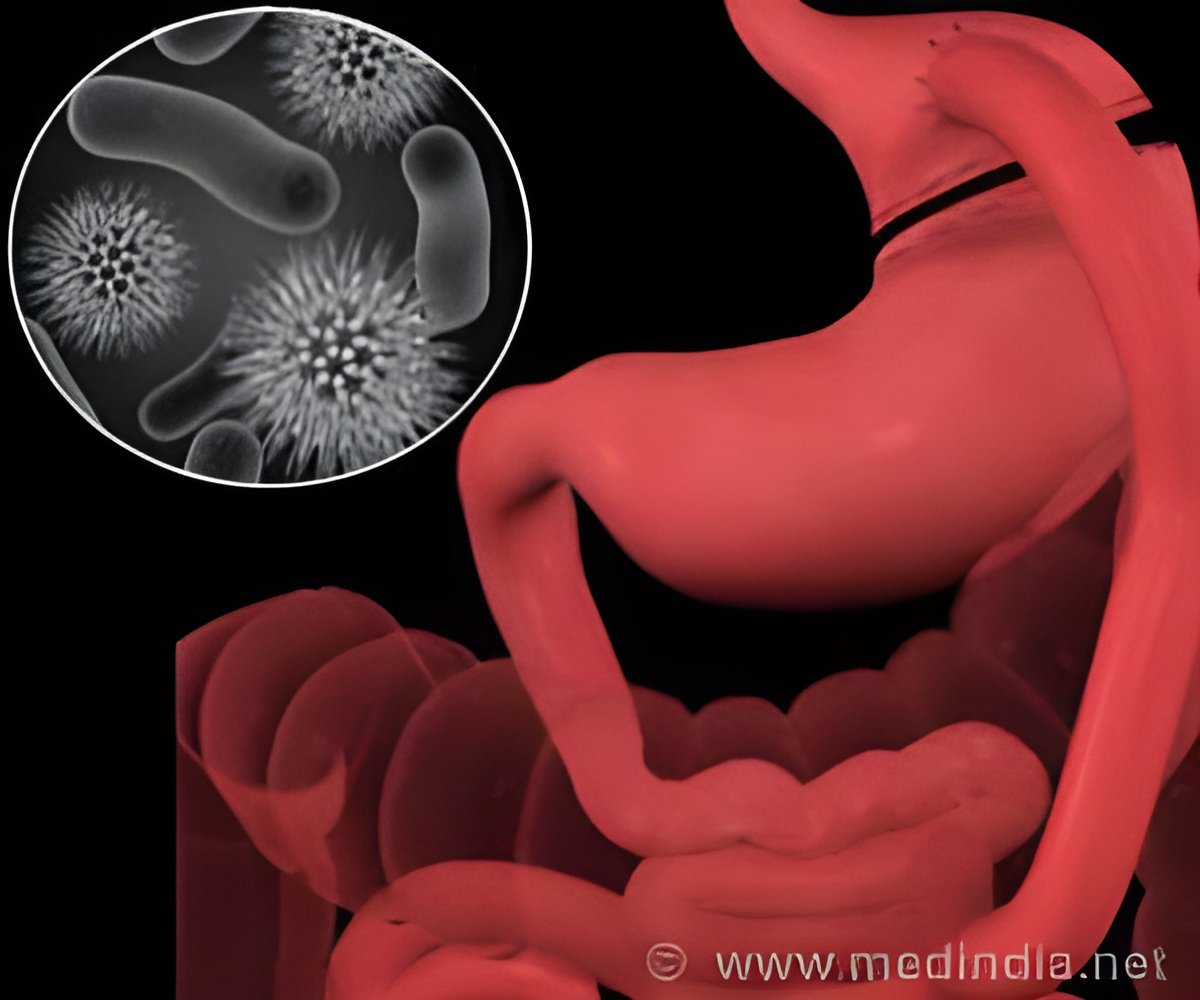
At the forefront of the defensive system is a layer of mucus that lines the entire gut surface.
In the large bowel, the mucus layer is an organised structure, with an inner layer that blocks bacteria, and an outer layer where beneficial bacteria (commensals) can flourish.
The mucus layer is made up of large proteins called mucins with characteristic sugary, or glycosylated, chains.
Advertisement
At the molecular level, mucins exhibit clusters of glycosylation that give the proteins a 'bottle-brush' appearance.
Advertisement
A myriad of different conformations that the sugar chains can take up means that mucins are incredibly diverse.
The differences are believed to help commensal bacteria by providing specific binding sites, as well as necessary nourishment.
Pathogenic bacteria have also evolved mechanisms to bind to mucins, as part of their arsenal to overcome our defences.
We, however, are a long way behind these bacteria in understanding the coded information contained in these complex sugar chains.
Understanding this "glycocode" would give us a new way to look at the crucial interactions between good and bad microorganisms in our guts, and may also provide new insights into gut diseases.
These interactions happen at the molecular level, so for us to understand them we need tools that work at this level.
IFR has a history of pioneering use of one such tool, atomic force microscopy (AFM).
AFM combines very high-resolution imaging with an ability to probe the forces between molecules.
AFM works by running a very fine stylus (tip) mounted on the end of a flexible cantilever over the surface of a molecule, much like a blind person reading braille.
A laser is bounced off the cantilever, amplifying the signal so that AFM can detect distances down to a millionth the width of a sheet of paper.
Patrick Gunning and Andrew Kirby, from IFR's AFM group, adapted this technique by attaching sugar-binding molecules called lectins to the AFM cantilever, via a flexible linker. They used this to probe mucins bound to a surface.
Schematic diagram showing a mucin molecule being probed by a lectin bound to an AFM cantilever. When the lectin 'snags' on sugar, the cantilever registers this.
The spatial arrangement of these signals can be used to fingerprint the mucin.
Measuring the distance between the snags gives a picture of what the overall mucin molecule looks like.
By repeating this thousands of times, and then working with IFR's biomathematicians, it was possible to produce a 'fingerprint' that characterise different mucins, which means that we could differentiate between mucins derived from different parts of the gut.
The researchers now want to look at the mucins derived from diseased tissues, to further investigate differences in the glycocode.
The findings were published in the FASEB Journal.
Source-ANI