Thompson, Northwestern's Ralph and Jean Sundin Professor of Communication Sciences, will participate in a 10 a.m. media briefing on "Tools for Regaining Speech" in Room 103 of Boston's Hynes Convention Center. The "Teaching the Brain to Speak Again: New Frontiers in Trauma and Stroke Recovery" panel takes place in Room 304 from 3 to 4:30 p.m.
For three decades, Thompson has played a crucial role in demonstrating the brain's plasticity, or ability to change. "Not long ago, the conventional wisdom was that people only could recover language within three months to a year after the onset of stroke," she says. "Today we know that, with appropriate training, patients can make gains as much as 10 years or more after a stroke."
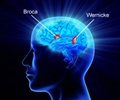
Thompson has probably contributed more findings on the effects of brain damage on language processing and the ways the brain and language recover from stroke than any other single researcher. Her particular interest is agrammatic aphasia, which impairs abstract knowledge of grammatical sentence structure and makes sentence production and understanding difficult.
Among the first researchers to use functional magnetic resonance imaging to study recovery from stroke, Thompson found that behavior treatment that focused on improving impaired language processing affects not only the ability to understand and produce language but also brain activity.
She found shifts in neural activity in both cerebral hemispheres associated with recovery, with the greatest recovery seen in undamaged brain regions within the language network engaged by healthy people, albeit regions recruited for various language activities.
Advertisement
Thompson will discuss research she will conduct as principal investigator of a $12 million National Institutes of Health Clinical Research Center award to study biomarkers of recovery in aphasia.
Advertisement
In a landmark 2010 study, she and colleagues discovered two critical variables related to understanding brain damage recovery. They found that stroke not only results in cell death in certain regions of the brain but that it also decreases blood flow (perfusion) to living cells that are adjacent (and sometimes even distant) to the lesion.
Until that study, hypoperfusion (diminished blood flow) was thought only to be associated with acute stroke. Her team also found that greater hypoperfusion led to poorer recovery.
Source-Eurekalert