However, the team of investigators discovered during their analysis that as previously disabled optic nerve axons — that can lead to vision loss — recover, the remaining areas of permanent visual loss in one eye coincide with the areas that can still see in the other eye. The team found that the visual field of the two eyes fit together like a jigsaw puzzle, resulting in much better vision with both eyes open than could possibly arise by chance.
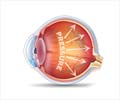
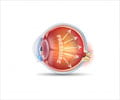
"As age and other insults to ocular health take their toll on each eye, discrete bundles of the small axons within the larger optic nerve are sacrificed so the rest of the axons can continue to carry sight information to the brain," explains author William Eric Sponsel, MD, of the University of Texas at San Antonio, Department of Biomedical Engineering. "This quiet intentional sacrifice of some wires to save the rest, when there are decreasing resources to support them all (called apoptosis), is analogous to pruning some of the limbs on a stressed fruit tree so the other branches can continue to bear healthy fruit."
According to the researchers, the cellular process used for pruning small optic nerve axons in glaucoma is "remarkably similar to the apoptotic mechanism that operates in the brains of people afflicted with Alzheimer's disease."
"The extent and statistical strength of the jigsaw effect in conserving the binocular visual field among the clinical population turned out to be remarkably strong," said Sponsel. "The entire phenomenon appears to be under the meticulous control of the brain."
The TVST paper is the first evidence in humans that the brain plays a part in pruning optic nerve axon cells. In a previous study, Failure of Axonal Transport Induces a Spatially Coincident Increase in Astrocyte BDNF Prior to Synapse Loss in a Central Target, a mouse model suggested the possibility that following injury to the optic nerve cells in the eye, the brain controlled a pruning of those cells at its end of the nerve. This ultimately caused the injured cells to die.
Advertisement
"This is consistent with the partial recovery of more diffuse overlapping visual field defects observed by Dr. Sponsel that helped unmask the more permanent interlocking jigsaw patterns once the eyes of his severely affected patients had been surgically stabilized," said Calkins.
Advertisement
Authors of the TVST paper suggest their findings can assist in future research with cellular processes similar to the one used for pruning small optic nerve axons in glaucoma, such as occurs in the brains of individuals affected by Alzheimer's.
"If the brain is actively trying to maintain the best binocular field, and not just producing the jigsaw effect accidentally, that would imply some neuro-protective substance is at work preventing unwanted pruning," said co-author of the TVST paper Ted Maddess, PhD, of the ARC Centre of Excellence in Vision Science, Australian National University. "Since glaucoma has much in common with other important neurodegenerative disorders, our research may say something generally about connections of other nerves within the brain and what controls their maintenance."
Source-Eurekalert