‘Inflammatory bowel disease (IBD) affects more than 1.6 million people in the U.S. Current therapies for IBD patients lead to remission in only about 30 percent of cases.’
Tweet it Now
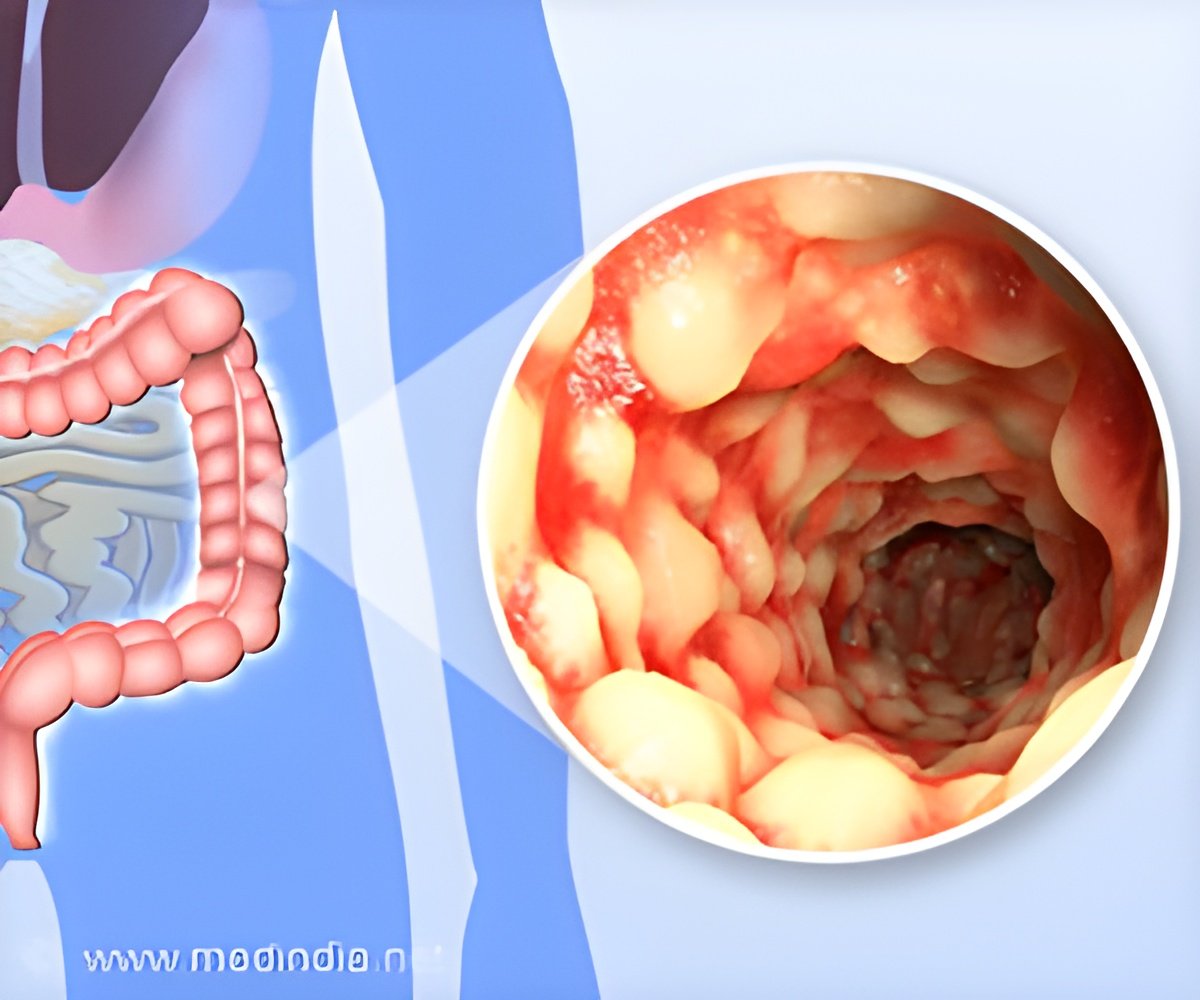
Investigators found that the beneficial effects of Bacteroides fragilis bacterium, one of billions of microscopic organisms that normally inhabit the human gastrointestinal system, were negatively impacted by variations in the ATG16L1 gene. These genetic variations increase the risk of developing Crohn's disease, one of the two common forms of IBD. As a result, the bacteria were prevented from carrying out one of their critical functions: suppressing inflammation of the intestinal lining. "This study is very important because it identifies a completely novel mechanism through which these genes may lead to an increased risk of developing Crohn's disease," said McGovern, director of the Precision Medicine Initiative at Cedars-Sinai. Using mouse models and human specimens, this study focused on Crohn's disease. Patients with this condition suffer from inflammation of the gastrointestinal tract, often resulting in severe abdominal pain and weight loss as well as symptoms outside the gut, including arthritis.
"Given the low percentage of IBD patients who respond to drugs directed at the immune system, these results could point the way to improving treatment by identifying patients who might best respond to manipulation of bacteria in their digestive tract," said study co-author Stephan R. Targan, MD, director of the F. Widjaja Foundation Inflammatory Bowel and Immunobiology Research Institute. The findings have implications for treating Crohn's disease as well as other immune disorders that share similar genetic variations.
"This study significantly advances the knowledge base for physicians treating patients with Crohn's disease. It also exemplifies the multidisciplinary endeavors under way at Cedars-Sinai to translate basic science discoveries to meaningful help for patients enduring the various challenges of inflammatory bowel disease," said Shlomo Melmed, MB, ChB executive vice president, Academic Affairs, and dean of the medical faculty at Cedars-Sinai.
Current therapies for IBD patients lead to remission in only about 30 percent of cases. Cedars-Sinai is at the forefront of research to pinpoint the role of genetics in the health of the digestive tract. This work is a critical step in developing specific therapies that can provide more effective and individualized treatments for patients. Inflammatory bowel disease (IBD) affects more than 1.6 million people in the U.S. Current therapies for IBD patients lead to remission in only about 30 percent of cases.
Advertisement