Investigators at Beth Israel Deaconess Medical Center and the Universite Libre de Bruxelles found patients with focal segmental glomerulosclerosis (FSGS) and hypertension-attributed end-stage kidney disease (H-ESKD) had variants in the APOL1 gene that changed the APOL1 protein sequence.
"We found that the APOL1 risk genes for renal disease occur in more than 30 percent of African-American chromosomes," co-senior author Martin Pollak of Harvard Medical School said in a statement.
"In fact, the increased risk of kidney disease in individuals who inherited two copies of these variant forms of APOL1 is reported to be approximately 10-fold."
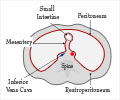
FSGS is an injury to the kidney's filtering system and ESKD indicates a kidney failure so severe the patient needs dialysis or a kidney transplant.
Kidney problems, which see about half a million US patients require dialysis treatment to replace their failed organs, are particularly pronounced among African-Americans.
Using information from the 1000 Genomes Project DNA data bank, the researchers singled out candidate genetic variants and tested DNA sample sets for their presence.
They found that the APOL1 variants G1 and G2 were linked to a greater risk of both FSGS and hypertension-attributed ESKD in African-Americans.
"G1 and G2 both changed the coding sequence of APOL1," explained Pollak. "Further analyses revealed that these very same genetic variants conferred human immunity against the parasite responsible for sleeping sickness."
The tsetse fly transmits the African trypanosome parasite, which causes sleeping sickness. The disease, not found outside Africa, causes severed nervous system disorders and can ultimately lead to brain damage, coma or death.
Source-AFP