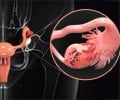
Researchers said Wednesday they have identified two new genetic mutations linked to the deadliest types of ovarian cancer. The discovery could pave the way for new therapies, it is hoped.
Scientists at the Johns Hopkins Kimmel Cancer Center hope their research will help develop treatments and drugs that will better target ovarian clear-cell carcinoma, which accounts for about 10 percent of cancers that start in the cells on the surface of the ovaries.
The disease mainly affects women aged 40 to 80 and resists chemotherapy.
Writing in the journal Science, a team of researchers led by Bert Vogelstein named the two genes as ARID1A and PPP2R1A, which have not been previously linked to ovarian cancer.
"They may provide opportunities for developing new biomarkers and therapies that target those genes," said Nickolas Papadopoulos, an associate professor of oncology at Johns Hopkins.
ARID1A mutations were identified in more than half of tumors studied.
"This gene may play a significant role in this type of cancer," noted Sian Jones, a Johns Hopkins research associate.
For their study, the scientists screened mutations in 18,000 protein-encoding genes in ovarian clear-cell tumors from eight patients at Johns Hopkins and institutions in Japan and Taiwan.
They purified the cancer cells and evaluated genes from those cells as well as from normal cells found in the same patients' blood or uninvolved tissues.
Among the eight tumors, the researchers found 268 mutations in 253 genes, or an average of 20 mutations per tumor. They then identified ARID1A mutations in 57 percent of 42 tumors of 34 additional ovarian clear-cell cancer patients.
PPP2R1A mutations were found in 7.1 percent of the tumors.
In a separate study published in the New England Journal of Medicine and focusing on ARID1A, Canadian researchers led by David Huntsman of the British Columbia Cancer Agency came to similar conclusions.
They found the gene was mutated in both ovarian clear-cell carcinoma and another type of ovarian tumor linked to endometriosis, a condition in which cells that usually line the uterus grow in other areas, often on the ovaries.
"Overall, 46 percent of patients with ovarian clear-cell carcinoma and 30 percent of those with endometrioid carcinoma had... mutations in ARID1A," the researchers said, noting they did not find the mutation in other types of ovarian tumors.
They said the gene was also suspected of playing a role in certain types of breast and lung cancer.
the World Health Organisation.
Source-Medindia