When used to treat a disease, human stool constitutes a drug and a biologic. Therefore, an investigational new drug approval was obtained from the United States Food and Drug Administration (FDA) to utilize FMT for treating ulcerative colitis in this trial.
The study results have been published online by the Journal of Pediatric Gastroenterology & Nutrition and will be featured in the June print edition.
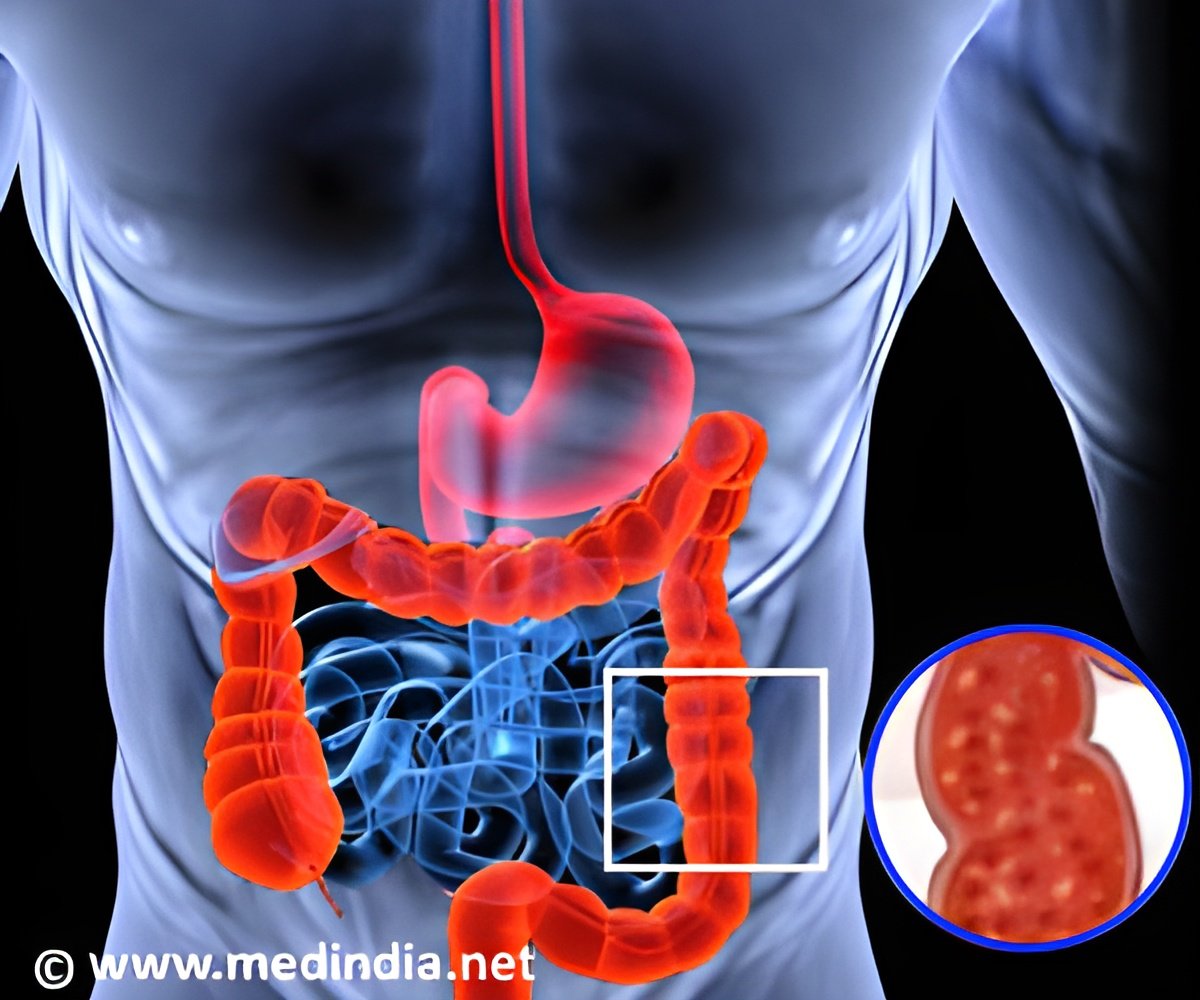
"FMT has been proposed as a promising new treatment option for recurrent C. difficle infection and possibly for ulcerative colitis as well," said Sachin Kunde, MD, MPH, pediatric gastroenterologist, Spectrum Health Medical Group, and lead investigator. "We believe that the procedure may restore 'abnormal' bacteria to 'normal' in patients with ulcerative colitis. Our short-term study looked at the safety and tolerability of FMT for these patients." According to the National Institutes of Health, ulcerative colitis is a type of inflammatory bowel disease (IBD) that affects the lining of the large intestine, or colon, and rectum. Symptoms can present slowly or occur suddenly and include abdominal pain, cramping, bloody diarrhea, pus in the stool, fever, rectal pain, weight loss, nausea, vomiting, joint pain, mouth sores or skin lesions and slow growth in children. For children, the disease often means missing school and curbing social activities which can lead to isolation from peers. This can be a significant psychological burden on children and their families.
Dr. Kunde explained that this single-center pilot study enrolled 10 children and young adults, ages 7-20 years, with mild to moderate ulcerative colitis. Lab-prepared stool samples from a healthy adult donor were infused via enema daily for five total infusions, scheduled within one week.
Clinical response was evaluated with the Pediatric Ulcerative Colitis Activity Index (PUCAI) score which measures disease activity of ulcerative colitis. Clinical response to FMT was defined as decrease in the PUCAI score by 15 points. These scores were collected at baseline and weekly for four weeks after transplantation.
Advertisement
"Patients often face a tough choice between various medications that have significant side effects. Allowing the disease to progress can lead to surgical removal of their colon," said Dr. Kunde. "Our study showed that fecal enemas were feasible and well-tolerated by children with ulcerative colitis. Adverse events were mild to moderate, acceptable, self-limited, and manageable by patients."
Advertisement
"We must further investigate standardization of FMT preparation, ideal donor selection, the best route of administration, and optimal duration or scheduling of FMT to induce and maintain a clinical response."
Dr. Kunde also explained that one of the challenges is to create awareness so that FMT is a socially and medically acceptable option. Subjects in the study did not see, smell or have any physical contact with fecal material other than receiving it as an enema, which decreased their anxiety and uneasiness towards the treatment.
"This study opens the doors for an innovative, inexpensive and natural alternative to improve outcomes of this debilitating disease with billions of dollars in health care cost," said Dr. Kunde. "However, we are still in very early stages of this field and need more evidence in terms of scientifically robust multicenter clinical trials before we can offer this to patients on clinical basis. Caution must be taken that FMT should be offered by centers that follow regulatory guidelines around this new therapy and have facilities and resources available to perform the procedure."
Source-Eurekalert