Statins could have their side-effects. But better grin and bear them if you want to survive. Such seems to the message of a study carried out in Spain.
Researchers found that the chances of dying, or requiring full-time care were nearly five times higher if statins were interrupted.The article, in the journal Neurology, advises doctors to continue giving the drugs to stroke patients.
But experts called for bigger studies before recommendations be made.
A UK stroke consultant pointed out that almost a third of stroke patients would find it too hard to swallow the pills.
The news follows a British Medical Journal report that found the UK lags behind the rest of western Europe in terms of stroke care.
Strokes are the third most common cause of death in the UK, accounting for more than 60,000 deaths a year.
Advertisement
Many people at high risk of stroke will be at higher risk of heart disease, and may be taking statins as a result.
Advertisement
However, the latest study, from the University of Santiago de Compostella, found a huge difference in the outcome for patients who were allowed to carry on taking their statins when they reached hospital after a stroke.
They followed the progress of 89 stroke patients who were already taking the drugs.
For the first three days after the stroke, 46 patients received no statins, and 43 got their normal dose.
After three months, 27 people - 60 % of the "no statins" group - had either died or were disabled to the point that they needed help to live a normal life, compared with 16 people from the group allowed to keep taking statins.
Lead researcher Jose Castillo said: "These results strongly support the recommendation to physicians to continue statin drugs during the acute phase of an ischaemic stroke."
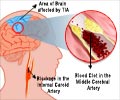
(Ischaemic (or ischemic) heart disease results from reduced blood supply to the heart. Ischaemia means a "reduced blood supply". The coronary arteries supply blood to the heart muscle and no alternative blood supply exists, so a blockage in the arteries reduces the supply of blood to heart muscle.)
However, consultant stroke physician Dr Anthony Rudd, from Guys' and St Thomas' Hospital in London, said that the evidence about the benefits of statins in stroke patients was contradictory.
He said: "This is a very small study, and I think we'd need to see bigger studies before drawing any firm conclusions."
He said that hospitals generally allowed patients to continue with their existing medication where possible, but added: "One practical problem is that up to 30% of stroke patients have difficulty swallowing, and it may prove difficult for them to continue taking their tablets normally."
The most common side effects of statins are headache, nausea, vomiting, constipation, diarrhea, rash, weakness, and muscle pain. The most serious (but fortunately rare) side effects are liver failure and rhabdomyolysis.
Rhabdomyolysis is a serious side effect in which there is damage to muscles. It often begins as muscle pain and can progress to loss of muscle cells, kidney failure, and death.
Naturally many are frightened away from this class of drugs. But the point is not to run away but to take appropriate medical counseling, it is suggested.
Source-Medindia
GPL/C