"Patients with obesity and Type 2 diabetes should consider these long-term results when making decisions about their weight loss treatment," Simonson said.
The researchers evaluated the effects of weight loss on 38 patients' self-reported health status for both physical and mental health, as well as the impact of their weight on their quality of life and on problem areas in managing their Type 2 diabetes.
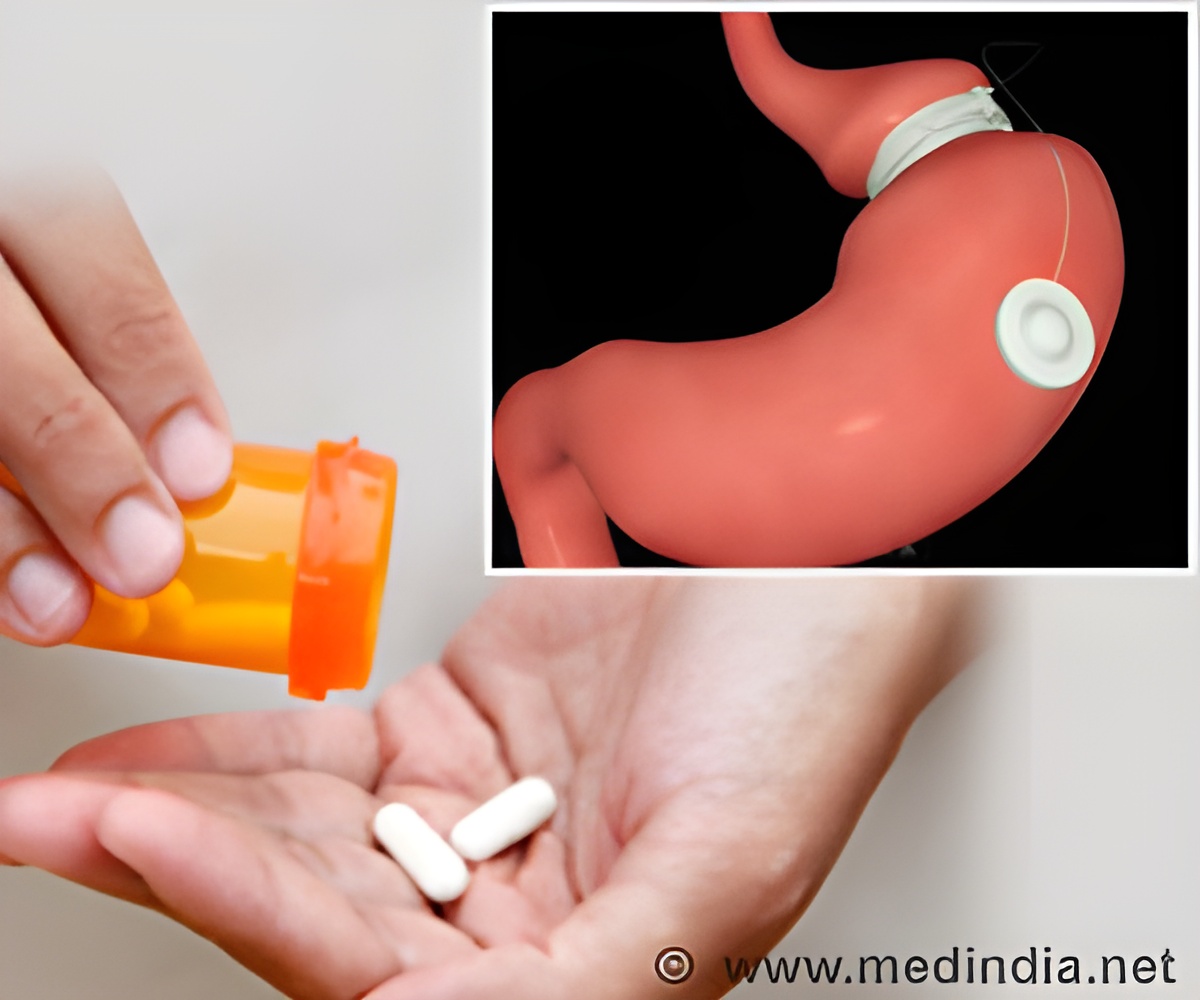
Fifteen men and 23 women participated in the Surgery or Lifestyle with Intensive Medical Management in the Treatment of Type 2 Diabetes (SLIMM-T2D) trial. Of the 38 patients, 19 were randomly assigned to undergo gastric bypass surgery at Brigham and Women's Hospital, and 19 patients, to a medical diabetes and weight management program, called Why WAIT (Weight Achievement and Intensive Treatment), at the Joslin Diabetes Center in Boston. The program consisted of exercise, diet with meal replacements, 12 initial weekly group sessions and nine additional months of individual counseling. Follow-up evaluation ranged from 18 to 24 months.
Before treatment, patients reported high scores on the questionnaire Impact of Weight on Quality of Life, which included physical function, self-esteem, sex life, public distress and work. Up to two years after treatment, patients who underwent gastric bypass surgery had nearly twice the improvement (reduction) in the adverse effects of weight on their quality of life, which Simonson said strongly correlated with the greater amount of weight they lost.
Two years after treatment, the surgical patients lost an average of 64.4 pounds versus 11 pounds in the Why WAIT group, he noted.
Advertisement
Although the Why WAIT program improved self-reported physical and mental health more than gastric bypass did at three months, improvements were generally similar in the two groups after one and two years of follow-up and were in the moderate range, Simonson reported.
Advertisement