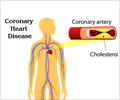
Here’s another reminder to those frivolous with their health. A new study has suggested that although new and improved treatment options are available to boost survival rates of coronary heart disease patients, the remainder of their lives may be less than satisfactory. The quality of those extra years may be less than ideal, they add.
Adults with cardiovascular trouble scored up to 9 percent lower on four scales measuring their quality of life, when compared with adults without coronary heart disease (CHD).Lead author Jipan Xie, M.D., Ph.D., former health scientist in the Division for Heart Disease and Stroke Prevention at the Centers for Disease Control and Prevention in Atlanta, Ga, said that patients with coronary heart disease were more likely to say they had poorer quality of life, or describe themselves as sick.
Those most likely to report poorer quality of life in this study were between the age group of 18 to 49; women; and black or Hispanic.
Xie said that the age-related difference probably reflects a difference in age-related expectations.
"Younger people may feel more pressure - especially younger men - in the workplace and may be more threatened by limitations imposed by their disease," she said.
Older people, especially those who were older than 65, were less likely to say heart disease limited their life or had an adverse effect on their quality of life.
Advertisement
For the study, researchers used data from the 2000 and 2002 Medical Expenditure Panel Surveys and they identified 2,091 people with a history of coronary heart disease from a sample of 37,386 individuals.
Advertisement
Researchers noted that men and women with heart disease rated lower on the mental health measure than did participants free of CHD.
Yet, while self-rated health scores indicated that men were more affected by CHD than women, physical health scores indicated women with heart disease had more functional impairment than men.
Xie said contradictory findings are fairly common in these types of analyses, but the findings suggest a disconnect between self-perception and functional ability.
Researchers said the study is limited because the disease status was self-reported and patients had various stages of CHD and treatments.
Also, there was not enough information to explain the differences in patient-reported health status among demographic subgroups.
The study is published in Circulation: Journal of the American Heart Association.
Source-ANI
TAN/M