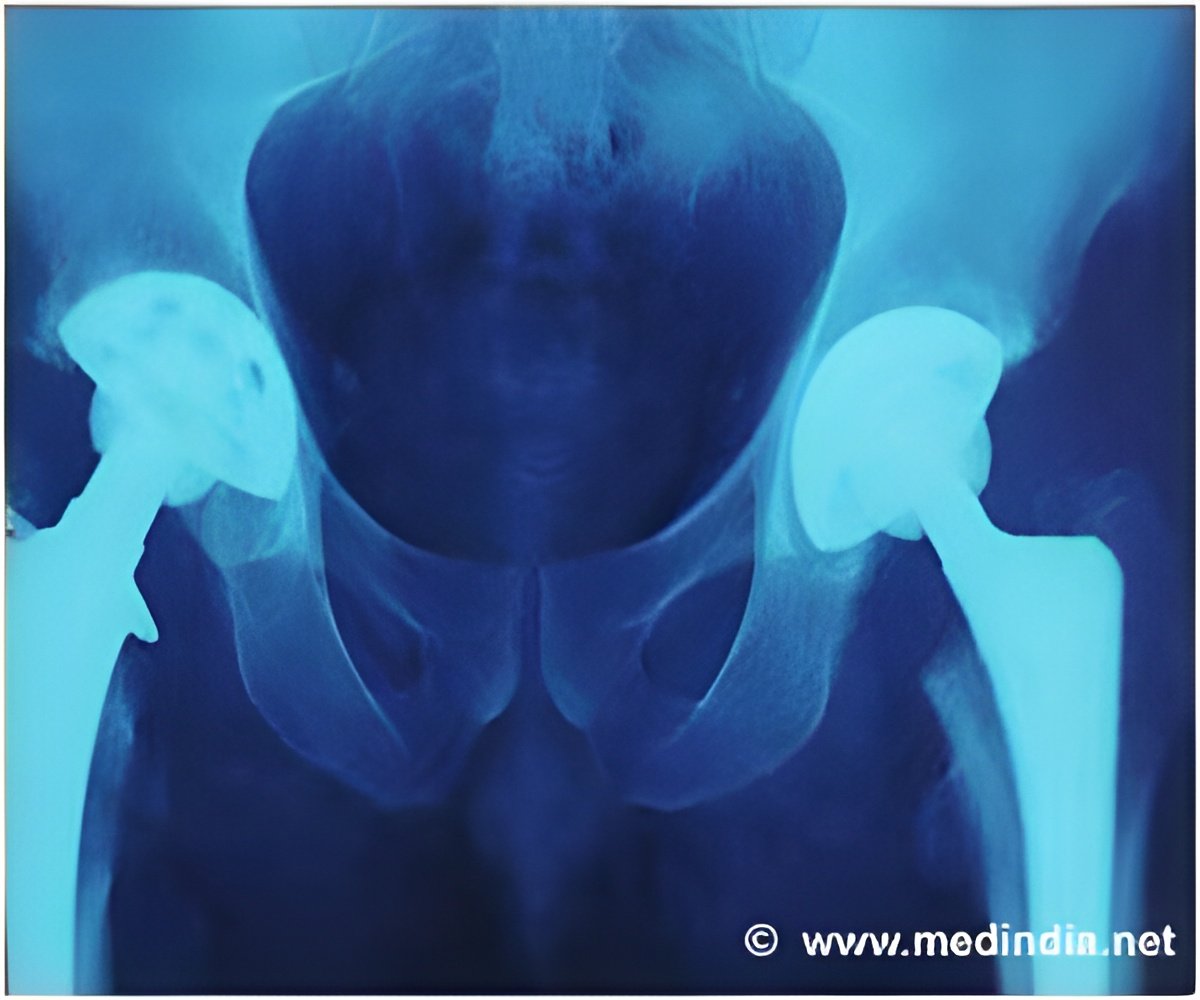
Oral bisphosphonates are used to prevent fractures and to treat common bone diseases like osteoporosis. Some experts think that bisphosphonates may improve the survival time of replacement joints through their effects on reducing bone resorption, but evidence is scarce and controversial.
So a team of researchers, led by Professor Nigel Arden at the University of Oxford, set out to test whether bisphosphonate use is related to improved implant survival time.
Using data from the General Practice Research Database, which contains anonymised data on three million UK primary care patients, they identified all patients over the age of 40 undergoing hip or knee replacement surgery from 1986-2006 for osteoarthritis.
Patients who were prescribed bisphosphonates at least six months before revision surgery were defined as bisphosphonate users. Non-users were defined as those who were never prescribed bisphosphonates or who had their first prescription after revision surgery.
Factors that could affect the results, such as age, sex, body mass index (BMI), smoking status, alcohol intake, use of calcium and vitamin D supplements, and previous fractures were also taken into account.
Advertisement
Bisphosphonate users had a lower rate of revision rate at five years than non-users. Bisphosphonate use was associated with an almost twofold increase in implant survival time.
Advertisement
And they suggest that the results could be due to bisphosphonate therapy suppressing the long term inflammatory response around the implant after surgery that often leads to bone loss and loosening of the implant.
Further studies are needed to confirm these findings, write the authors. However, they say that the protective effect of bisphosphonates seen in this study can be assumed to be valid for the wider population of patients undergoing total hip or knee replacement in the UK.
Source-Eurekalert