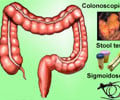
Colorectal cancer (CRC) has a very high incidence in Switzerland as well as in other European countries and is the second most frequent cause of cancer-related deaths in Europe. It is detected in approximately 413,000 people in Europe every year, half of whom die because of the disease. Therefore a need exists for efficient strategies for prevention and early detection of CRC. Colonoscopy with the possibility of an immediate polypectomy is a recommended and preferred screening method because polyps (growths in the colon) can turn into cancer over the course of years to decades. Removing polyps during a colonoscopy prevents that polyp from becoming cancerous.
"In contrast to earlier CRC screening studies that used colonoscopy, this population-based closed cohort observational study aimed to obtain complete and comparable data on CRC incidence and CRC-related mortality after a single screening colonoscopy compared with no screening, while taking into account the potential differences in risk profiles between the screened and non-screened participants," said study lead author Urs A. Marbet, Cantonal Hospital of Uri, Altdorf, Switzerland. "We found that colorectal cancer screening by colonoscopy markedly reduces not only the incidence of colorectal cancer, but also cancer-related death. We are unaware of any other long-term prospective study assessing the role of colonoscopy screening for the reduction of colorectal cancer incidence and mortality in a well-defined, population-based setting under real-life conditions."
MethodsThe researchers' objective was to compare the incidence of and mortality from CRC among individuals screened by colonoscopy and non-screened individuals. The study involved 1,912 screened patients and 20,774 non-screened control participants. It was a closed cohort study in a population-based setting in a precisely defined area with a low level of population migration (a mainly rural area of Switzerland) from June 1, 2000 to June 1, 2001. Colonoscopies were performed by 11 board-certified gastroenterologists,including three local gastroenterologists who were supported by 10 gastroenterology trainees from the University Hospitals of Basel and Zurich; each of the trainees had performed at least 200 procedures. Study participants were aged 50 to 80 years old.
CRC cases in this closed cohort study were prospectively collected during the screening period of one year and the follow-up period of six years (June 1, 2001 to May 31, 2007). The main outcome measurements included follow-up data that were corrected for negligible migration balance in the area, and included tumor characteristics and risk or protective factors, age and sex, participation in general health screening examinations, history of CRC in a first-degree relative, smoking status, body mass index, frequency of sports activity, eating habits, and patients' professions. Colorectal cancer and cancer-related death was recorded for all participants. Statistical comparisons were made between the screened and non-screened patient groups.
ResultsPolyps were found in 565 of the 1,912 screened individuals (29.6 percent), including 374 persons (19.6 percent) with adenomas (precancerous polyps) by histology. All polyps found during colonoscopy were removed during the procedure, except for very small lesions in the rectum, or later by surgery (surgical polyp removal occurred in seven cases -- 0.36 percent). Overall, 1,279 polyps were removed. Colorectal cancer incidence was significantly reduced by colonoscopy screening. Overall, 225 colorectal cancers were detected. A total of 12 CRC cases were found in the screened group (0.6 percent of the screened persons), including one which was found during follow-up 60 months after the initial screening (0.05 percent of screened persons). In the non-screened group, there were 213 cases of CRC (1.0 percent). None of the non-screened patients, of whom five presented with synchronous cancers, and none of the persons who had been excluded from screening, had previously undergone a colonoscopy.
Advertisement
The researchers found in this closed cohort study a substantial reduction in the incidence of colorectal cancer and colorectal cancer–related mortality in a sample of asymptomatic individuals undergoing a single colonoscopy screening compared with non-screened individuals.
Advertisement
Source-Eurekalert