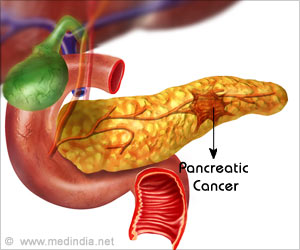
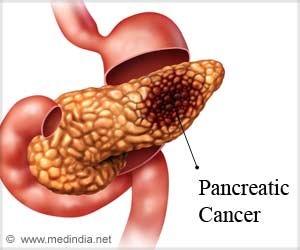
Patients who can undergo surgery as part of treatment often survive longer and some patients fare best when they can receive chemotherapy prior to surgery.
‘Pancreatic cancer patients who had three or four of the altered genes had worse disease-free survival and overall survival (from surgery to death), compared to patients with a single or two altered genes.’





For the study, published in the Journal JAMA Oncology, involved 356 patients who all had pancreatic adenocarcinoma that could be surgically removed. Adenocarcinoma is by far the most common type of pancreas tumour.
Ninety of the patients were treated at the University of Rochester Medical Centre's Wilmot Cancer Institute; the others at Dana Farber/Brigham and Women's Cancer Centre in Boston and Stanford Cancer Institute.
In all cases after the tumours were removed, scientists extracted DNA from the cancerous tissue and nearby normal tissue and conducted next-generation DNA sequencing on the specimens.
The analysis centred on the activity of the KRAS, CDKN2A, SMAD4, and TP53 genes.
Advertisement
Pancreatic cancer is aggressive and generally has poor survival odds.
Advertisement
Source-IANS