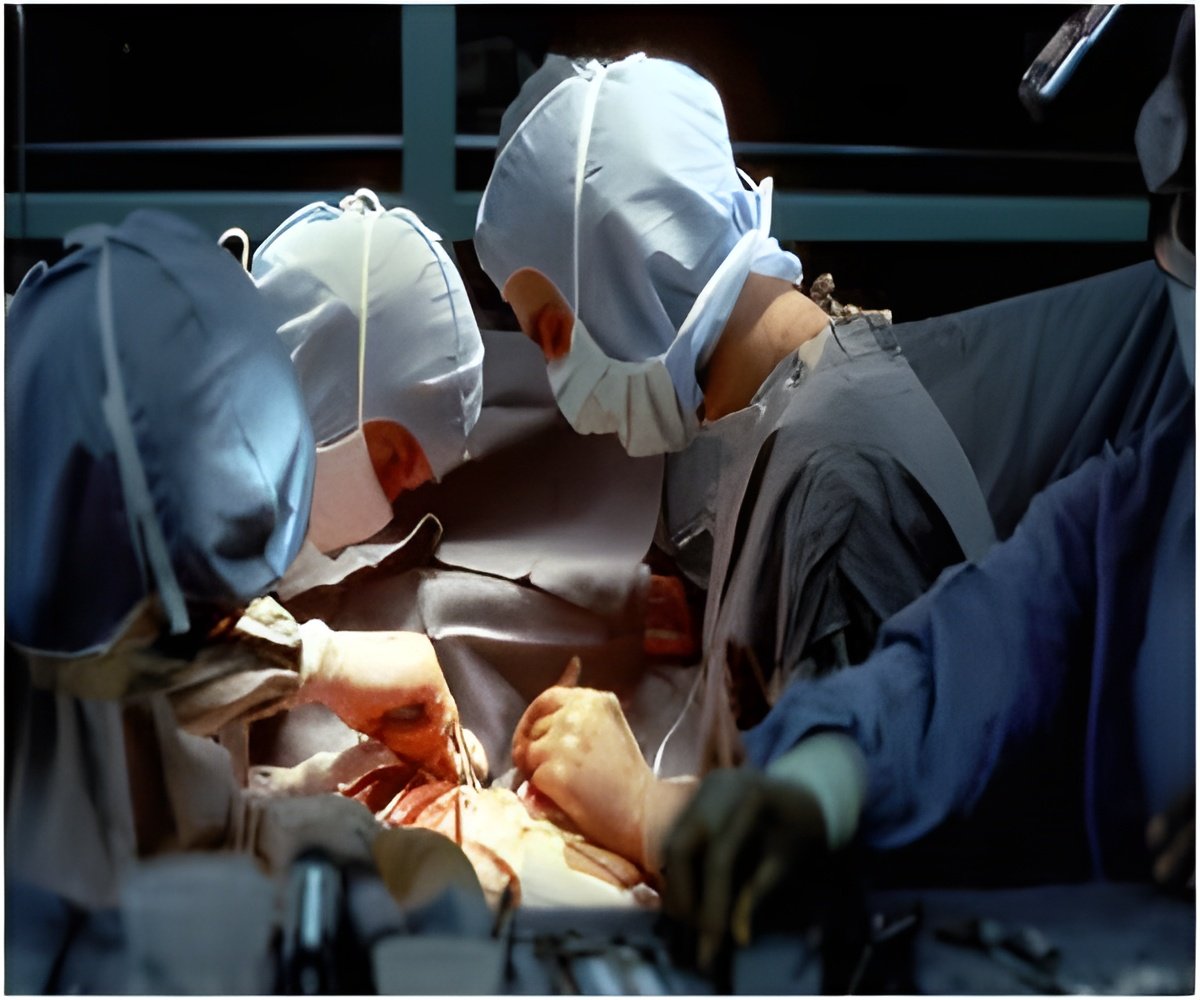
Globally, oesophageal cancer is the eighth most common form of cancer. The prognosis is a poor one, and only 10 per cent of patients survive five years after diagnosis. The disease is often discovered in a late stage after symptoms such as swallowing difficulties and weight loss appear. The only established curative treatment includes extensive surgery, often of the abdomen, chest and throat. Some 30 per cent of patients survive the operation at least five years. The purpose of the current study was to establish if the quality of life among five-year survivors of surgery for oesophageal cancer is on a par with that of the average population.
The study included 117 patients who had undergone surgery for oesophageal cancer in Sweden between 2001 and 2005, and survived at least five years. The patients were asked to answer a quality of life questionnaire that measured a range of functions (e.g. physical, social and emotional) and symptoms (e.g. pain, fatigue and eating difficulties). To obtain an idea of what their quality of life was like before the operation, the researchers had a group of 4,910 randomly selected individuals answer the same questions. The replies were then re-calculated as points on a 0-100 scale, where high scores for functions and low ones for symptoms were good. The analyses were adjusted for age, sex and medical state of health.
What they found was that most patients had an unchanged or even improved quality of life, and one that was comparable with that of the normal population. However, one in six patients experienced a considerable deterioration in quality of life, which was persistently much lower than that of the normal population at five years post-surgery. Physical function, for example, had remained unchanged or improved in 86 per cent of the patients, whose score on this factor was 87 five years after surgery, compared to 88 for the normal population; the corresponding score for the 14 per cent of patients who had deteriorated over the five years was 56.
"The patients who show early signs of impaired quality of life should be identified and helped through a more intensive follow-up to avoid a persistently low quality of life," says principal investigator Pernilla Lagergren, professor of surgical care sciences at the Department of Molecular Medicine and Surgery at Karolinska Institutet. Depending on the problems identified by the patients, targeted intervention is often possible. For example, a patient with particular nutritional problems can be referred to a dietician with specialist knowledge of this patient group.
Advertisement