Recent research from University of California has found that cancer patients of African-American descent are less likely to be seen by cancer specialists or receive cancer treatments.

The study, published online in the Journal of the National Cancer Institute, noted there was no difference in risk of death when black patients received the same treatments, such as chemotherapy and surgery, as non-Hispanic white patients.
"Other studies have looked at racial disparities in treatment and still others have focused on racial differences in survival rates of cancer patients, but our research attempted to go further by demonstrating the impact of race-based inequalities in cancer treatment on survival rates of black colorectal cancer patients," said James D. Murphy, MD, MS, assistant professor and chief of the Radiation Oncology Gastrointestinal Tumor Service at UC San Diego Moores Cancer Center.
The researchers analyzed data from 11,216 patients over the age of 66 with stage IV colorectal cancer from the Surveillance, Epidemiology, and End Results (SEER)-Medicare database. The analysis compared patient consultation rates with cancer specialists as well as treatment with surgery, chemotherapy and radiation therapy for white and black patients.
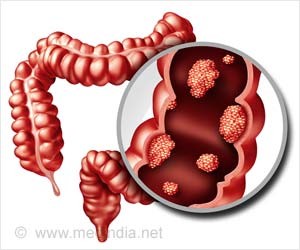
Despite screening efforts and improvements in treatment, colorectal cancer is the third leading cause of cancer death in the United States, according to the American Cancer Society, with approximately 50,000 deaths annually. This disease disproportionally affects black patients, with higher incidence rates, more advanced stage at diagnosis and decreased survival rates compared to other ethnic groups.
The study concluded that black patients were 10 percent less likely to have primary tumor surgery, 17 percent less likely to receive chemotherapy and 30 percent less likely to receive radiotherapy. Among patients who received chemotherapy, white patients were more likely to receive more than one chemotherapy agent. The researchers noted that black patients typically received chemotherapy four days later than white patients. Chemotherapy was associated with a 66 percent decreased risk of death.
Advertisement
The study did not ascribe a specific cause for the racial disparities but offered six possible explanations: conscious or unconscious provider biases; patient mistrust; health literacy; patient-physician communication breakdown; healthcare access barriers; and/or race-based differences in disease biology.
Advertisement
Source-Eurekalert