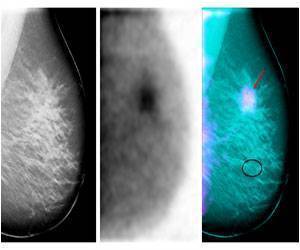
To learn whether CAD leads to more accurate reading of mammograms, Joshua J. Fenton, M.D., at the University of California, Davis, and colleagues analyzed data from more than 1.6 million film screening mammograms carried out at facilities in seven states from 1998 to 2006. The facilities participate in the Breast Cancer Surveillance Consortium, a federally supported network in which data quality is rigorously monitored.
Of 90 total facilities, 25 adopted CAD and used it for an average of 27.5 months during the study period. The researchers collected information on women who had mammograms with and without CAD, including whether they were diagnosed with breast cancer within a year of the screening.
According to the study, CAD was associated with more false positives—identifications of tumors that turned out to be false. It did not improve detection of invasive cancers. Moreover, the cancers detected using CAD were no more likely to be smaller or at a lower stage or to have less lymph node involvement than those detected without CAD. The results were the same after adjusting for patient age, breast density, use of hormone replacement therapy, and other factors that might influence mammography findings.
The authors point out that CAD costs Medicare more than $30 million a year. "As currently implemented in U.S. practice," they write, CAD appears to increase a woman's risk of being recalled for further testing after screening mammography while yielding equivocal health benefit."
In an accompanying editorial, Donald Berry, Ph.D., of the M.D. Anderson Cancer Center in Houston argues that any benefit to CAD is likely to be so small that it would be difficult to detect even in a very large randomized study. Moreover, improving the sensitivity of CAD might find less aggressive tumors or those that would otherwise show up between mammograms. Early detection of such tumors, he writes, is not likely to have much of an impact on breast cancer mortality.
Advertisement
Source-Eurekalert