Two new research papers say that the injections of the steroid corticosteroid triamcinolone may help restore vision in some patients with retinal vein occlusion. The latter is an important cause of vision loss that results from blockages in the blood vessels in the retina.
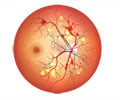
Retinal vein occlusion is an important cause of vision loss worldwide, according to background information in the articles published in the September issue of Archives of Ophthalmology.The condition frequently occurs in individuals with diabetes, and leads to macular edema, or fluid build-up in the retina.
Although a laser treatment of the retina called grid photocoagulation has shown a benefit in improving the vision of patients with blockages in smaller branches of the retinal vein, there is presently no effective therapy for vision loss associated with macular edema after central retinal vein occlusion-blockage in the main portion of the retinal vein, at the optic nerve.
One of the research papers reports the results of a randomised clinical trial involving 271 participants with macular edema from central retinal vein occlusion.
Ninety-two of the participants were assigned to receive 1 milligram of intravitreal (injected into the eye) triamcinolone, 91 received a 4-milligram dose and 88 were assigned to an observation group that did not receive treatment.
The participants were evaluated every four months for 12 months, and those in the triamcinolone group received additional injections at each follow-up visit unless there was a specific reason not to re-treat them. Additional follow-up data were collected annually through 36 months, although complete 24- and 36-month outcome assessments were not available for analysis.
Advertisement
The odds of reaching a predetermined level of visual improvement were five times greater among individuals receiving either dose of triamcinolone than those not receiving treatment.
Advertisement
"The superior safety profile of the 1-milligram dose compared with the 4-milligram dose, particularly with respect to glaucoma and cataract, renders it the preferred dose," the authors write.
Based on the results, the authors concluded: "Intravitreal triamcinolone in a 1-milligram dose and following the retreatment criteria used in this study should be considered for up to one year, and possibly two years, in patients with vision loss associated with macular edema secondary to central retinal vein occlusion who have characteristics similar to the participants studied in this trial."
The second study by the same research group compared the safety and efficacy of triamcinolone with standard care-grid photocoagulation in eyes without hemorrhage, or deferring photocoagulation until hemorrhage clears-for 411 patients with macular edema from branch retinal vein occlusion.
A group of 137 was assigned to receive standard care, 136 to receive a 1-milligram dose of intravitreal triamcinolone and 138 to receive a 4-milligram dose. Similar to the central retinal occlusion trial, participants were evaluated and re-treated as indicated every four months.
After one year, 29 percent of participants in the standard care group, 26 percent in the 1-milligram triamcinolone group and 27 percent in the 4-milligram group experienced improved vision.
"The rates of adverse events with respect to cataract surgery and elevated intraocular pressure were similar between the standard care and 1-milligram groups, but the potential for added risks of procedure-related complications in the 1-milligram group (as exemplified by the one case of endophthalmitis [inflammation inside the eye] reported in the 4-milligram group) suggests a superior safety profile for the standard care group," the authors write.
According to them, adverse event rates were higher in the 4-milligram group.
"Thus, current study results (up to 12 months and possibly up to 36 months) support grid photocoagulation as the continued standard of care for patients with decreased visual acuity associated with macular edema secondary to branch retinal vein occlusion who have similar characteristics to the cohort in this clinical trial.
The results of this trial also support the idea that grid photocoagulation, as applied in the current study, should be the benchmark against which other treatments for vision loss associated with macular edema secondary to branch retinal vein occlusion are compared in clinical trials," the authors concluded.
Source-ANI
RAS