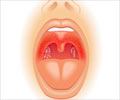
Sore throat, or pharyngitis, could be a sign of something worse like rheumatic fever, say scientists from the University of Alabama at Birmingham (UAB).
Currently, physicians are taught to suspect group A streptococcal bacteria as the primary cause of pharyngitis.However, new findings suggest that physicians also should look for the presence of bacteria called Fusobacterium necrophorum when treating sore throat in young adults and adolescents that worsens or is strep-negative.
"F. necrophorum, which only has been recognized as a potential cause of pharyngitis in adolescents and young adults in the past five years, may cause up to 10 percent of sore throat in those 15-24 years of age," Science Daily quoted Robert Centor, professor of internal medicine, associate dean of medicine at UAB and the paper's lead author, as saying.
"More important, F. necrophorum is associated with a rare but life-threatening complication called Lemierre syndrome," Centor added.
Lemierre syndrome mostly affects adolescents and young adults and rarely is seen in pre-adolescents. It begins with a sore throat, followed by an infected jugular vein after four to five days. Abscesses in other parts of the body may occur.
Group A strep also is associated with a serious complication - rheumatic fever - but the incidence rate of Lemierre syndrome following exposure to F. necrophorum is much higher and associated with greater morbidity and mortality.
Advertisement
Centor said that clinicians should expand their diagnostic process for adolescents and young adults with sore throat to consider F. necrophorum, especially if the sore throat does not improve within three to five days.
Advertisement
Aggressive treatment with antibiotics such as a combination of penicillin and metronidazole or with clindamycin alone is appropriate. Centor said he hopes this analysis will lead to better diagnostic tests for the presence of F. necrophorum.
The study has been published Dec. 1 in the Annals of Internal Medicine.
Source-ANI
TRI