In patients with type 2 diabetes, silent cerebral infarction (SCI)—small areas of brain damage caused by injury to small blood vessels—signals an increased risk of progressive kidney disease and kidney failure, according to a study appearing in an upcoming issue of the Journal of the American Society Nephrology (JASN).
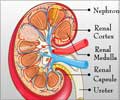
If SCI is present in the brain, it could be an indicator that small-vessel damage is present in the kidneys as well, suggests the new study by Takashi Uzu, MD (Shiga University School of Medicine, Otsu, Japan). Uzu comments, "Silent cerebral infarction may be a new marker to identify patients who are risk for declining kidney function."The study included 608 patients with type 2 diabetes, all initially free of symptomatic stroke, heart disease, or kidney disease (overt proteinuria or renal dysfunction). On magnetic resonance imaging (MRI) scans of the brain, 177 of the patients (29 percent) had SCI—subtle areas of brain damage caused by disease of the brain blood vessels, but not severe enough to cause overt symptoms of stroke.
At long-term follow-up, diabetic patients with SCI had higher risks of progressive kidney disease. Compared to those with normal brain MRI scans, patients with SCI were about 2.5 times more likely to die or develop end-stage kidney disease. Their risk of declining kidney function or dialysis was nearly five times higher.
New approaches are needed to assess the risk of diabetes-related kidney disease. "Microalbuminuria—small amounts of the protein albumin in urine—is the most important marker to predict the progression of kidney disease in diabetic patients," explains Uzu. "However, decreased kidney function without microalbuminuria is common in patients with type 2 diabetes."
The new study shows that diabetic patients with subtle brain damage detected on MRI scans are more likely to develop serious kidney disease, independent of microalbuminuria. "Evaluating both SCI and microalbuminuria may be useful for determining the risk of progression of kidney disease in diabetic patients," says Uzu.
The study had some risk of bias related to patient selection. Also, although most of the patients with SCI had multiple small areas of brain damage, the study did not exclude patients with relatively large areas of brain damage. "Therefore, not only small vessel disease but also relatively large vessel disease might have affected the progression of kidney disease in our patients," adds Uzu.
Advertisement
SRM