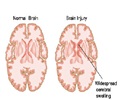
Researchers at the University of California-San Francisco (UCSF) have restored to normal levels a key protein that is involved in early brain development, and is linked to the rare brain disorder lissencephaly.
Reduced levels of the protein called LIS1 have been shown to cause lissencephaly, which is characterized by brain malformations, seizures, severe mental retardation and very early death in human infants.The findings in mice offer a proof-of-principle that the genetic equivalent to human lissencephaly, also known as "smooth brain" disease, can be treated during pregnancy and effectively reversed to produce more normal offspring.
The researchers are hoping that this approach could also be used to treat other defects in utero, or even those manifesting after birth, when caused by a partial deficiency in one gene, according to Dr. Anthony Wynshaw-Boris.
"Researchers have not considered it possible to treat such a pervasive, early developmental brain disorder as lissencephaly. Not only were we able to show a clear cellular effect from using these protease inhibitors, but also were able to treat the disorder in utero," Nature quoted Wynshaw-Boris as saying.
The work is the culmination of 15 years of collaborative research into the cause and mechanisms of lissencephaly, which is caused by a deletion or loss of one copy of the LIS1 gene, and affects an estimated one in 50,000-100,000 infants.
In 1998, the researchers reported of producing a mouse with the same mutation that displayed defective brain development.
Advertisement
The team then used a specific small-molecule protease inhibitor of calpain in these mice.
Advertisement
The team then gave daily injections of a calpain inhibitor to pregnant mice whose foetuses had the mouse-model of this defect.
They observed that the resulting offspring had more normal brains and showed no sign of mental retardation.
"This study is really a proof-of-principle not only for treating complex developmental brain disorders, but also for any disorder with reduced protein levels where proteases normally play some role in breaking down that protein. This will be much more difficult to apply to humans, because of the safety issues involved, but it could lead to new therapies that might be effective for a wide range of developmental disorders," said the researchers.
The findings have been published in the journal Nature Medicine.
Source-ANI
RAS