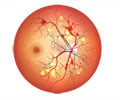
Researchers at the Medical College of Georgia believe the discovery of Interleukin-6, an inflammatory mediator key to the loss of vision caused by diabetic retinopathy, may help in the development of new treatment.
The study was conducted by Dr. Wenbo Zhang, assistant research scientist in MCG's Vascular Biology Center, Dr. Modesto Rojas, senior postdoctoral fellow and Dr. Ruth Caldwell, cell biologist a the Vascular Biology Center and the Charlie Norwood Veterans Affairs Medical Center.Zhang said: "We expect that this neutralizing antibody can be used to treat diabetic retinopathy in the future."
Angiotensin II, a powerful constrictor of blood vessels, plays an important role in regulating blood pressure in the kidneys. The scientists suspect angiotensin II also aids in wound healing and regulation of pressure within small blood vessels in the eye.
However in diabetes, angiotensin II levels rise in the eye, possibly in response to high glucose levels. The increased levels help promote inflammation, stimulating remodelling of blood vessels and tissue destruction.
Dr. Rojas said: "Vascular inflammation is one of the first steps to inducing the changes in the retina."
MCG scientists have demonstrated that interleukin-6 is a needed accomplice whose previously undetectable levels in the eye also increase, pointed out Caldwell.
Advertisement
The white blood cells also start producing inflammatory and vascular growth factors that cause blood vessel walls to leak and thicken, further reducing blood flow. Retinal cells start dying from the constricted blood and oxygen supplies that result. As a response, the body prompts growth of new blood vessels, probably to help but instead causing more vision impairment.
Advertisement
Rojas said: "Inflammation is a compensatory mechanism that gets activated as a survival mechanism...If it continues, the effect is bad."
Caldwell said: "We have known for along time if patients keep their blood sugar under perfect control, they don't have these problems, but that's hard.... That is why it's such a difficult disease."
To study interleukin-6's role in the destruction, the researchers injected angiotensin II into the vitreous portion of the eyes of mice missing the gene for the inflammatory factor as well as normal mice.
The extra angiotensin did not much affect the retinal vessels of mice lacking interleukin-6 but vessels in the normal mouse retina mimicked the inflammatory reaction found in diabetic retinopathy.
When interleukin-6 was reintroduced to the genetically altered mice, the damage mimicked that of the normal mice.
Caldwell said: "So when we knock out interleukin-6, we can block the effects of angiotensin II."
The research has been published online in Investigative Ophthalmology and Visual Science.
Source-ANI
SRM