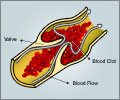
The clot builds up pressure and leaches inflammatory chemicals that can cause irreversible brain damage, often leading to death or extreme disability.
The usual treatments for ICH-either general supportive care such as blood pressure control and ventilation, which is considered the current standard of care, or invasive surgeries that involve taking off portions of the skull to remove the clot, have similar mortality rates, ranging from 30 to 80 percent depending on the size of the clot.
Seeking to improve these mortality rates and surviving ICH patients' quality of life, Daniel Hanley, M.D., professor of neurology at the Johns Hopkins University School of Medicine, and his colleagues developed and tested the new treatment on 60 patients at 12 hospitals in the United States, Canada, the United Kingdom and Germany.
After neurologists diagnosed patients in the treatment group with ICH at these hospitals, surgeons drilled dime-sized holes in patients' skulls close to the clot location.
Using high-tech neuro-navigational software that provides detailed brain images, the physicians threaded catheters through the holes and directly into the clots.
Advertisement
The researchers found that clot size in patients treated with either dose shrunk by more than half, compared to only 1 percent in patients who received only supportive care.
Advertisement
Those in the treatment group and the supportive care group had about a 10 percent mortality rate at 30 days after treatment, lower than the typically high mortality rates expected for this condition.
After following the patients out for six months, the researchers found that the treated patients scored significantly higher on a test that measures the ability to function in daily life compared to those who received supportive care.
Overall, Hanley says, the new treatment appears to be a viable and promising alternative to the current standard treatments of supportive care or invasive surgery.
"We're confirming that patients do recover better if we remove as much of the clot as we can, but gentle removal appears to be key," he said.
Adding: "Reducing the clot's size with a minimally invasive method seems to be pivotal for optimizing patient recovery."
Source-ANI