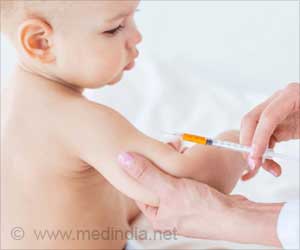
As a fetus does not mount an immune response to maternal proteins that cross the placenta, it has been assumed that a fetus would not reject non–genetically matched blood cells (specifically allogeneic blood cells) if they were transplanted while the fetus was in utero.
The hope is that this procedure, which is known as IUHCT, could provide a viable approach for treating congenital blood disorders. However, studies using a mouse model of IUHCT indicate that most fetal recipients of allogeneic blood cells lose their transplanted cells 3-5 weeks after transplantation.Alan Flake and colleagues, at Children's Hospital of Philadelphia, have now identified an immune mechanism responsible for graft failure in this model of IUHCT. Surprisingly, although fetal immune cells eliminated the transplanted allogeneic blood cells, they were triggered to do so by immune molecules known as alloantibodies that they obtained from their mother's breast milk.
The maternal alloantibodies were produced in response to IUHCT and so the authors conclude that in the absence of either a maternal immune response or transmission of the maternal alloantibodies to the fetus, transplanted blood cells should not be rejected, leaving open the door for IUHCT as a potential clinical strategy.
Source-Eurekalert
SRM