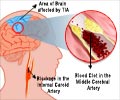
A new study has found that elevated nonfasting triglyceride levels, previously linked to an increased risk for heart attack, also appear to be associated with an increased risk for ischemic stroke.
Previous studies have found a strong link between elevated levels of nonfasting triglycerides, which indicate the presence of remnant (a small portion that remains) lipoproteins, and increased risk of ischemic heart disease."It is therefore possible that nonfasting triglyceride levels are also associated with increased risk of ischemic stroke," the authors said.
"Triglyceride levels are usually measured after an 8- to 12-hour fast, thus excluding most remnant lipoproteins; however, except for a few hours before breakfast, most individuals are in the nonfasting state most of the time.
"Therefore, by mainly studying fasting rather than nonfasting triglyceride levels, several previous studies may have missed an association between triglycerides and ischemic stroke," they added.
Jacob J. Freiberg, M.D., of Copenhagen University Hospitals, Denmark, and colleagues conducted a study to determine if increased levels of nonfasting triglycerides are associated with risk of ischemic stroke.
The Copenhagen City Heart Study, a Danish population-based study initiated in 1976 with follow-up through July 2007, included 13,956 men and women age 20 through 93 years.
Advertisement
Of the 13,956 participants in the study, 1,529 developed ischemic stroke. The researchers found that the cumulative incidence of ischemic stroke increased with increasing levels of nonfasting triglycerides.
Advertisement
The study is published in the November 12 issue of JAMA.
Source-ANI
SK